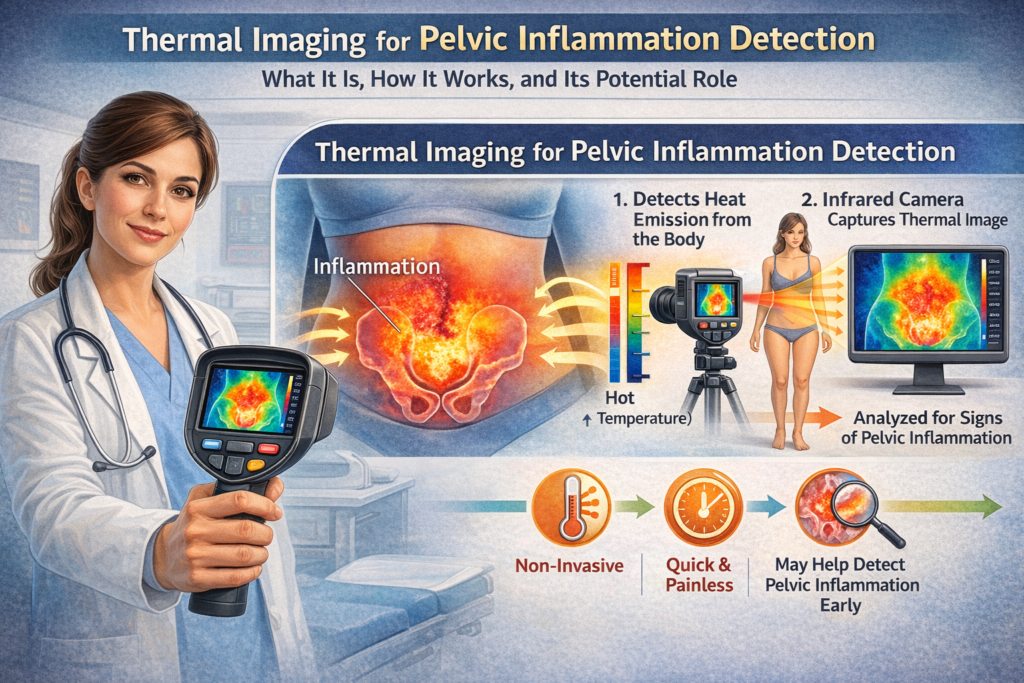
Thermal imaging, also known as infrared thermography (IRT) or digital infrared thermal imaging (DITI), is a non-invasive, radiation-free technique that detects and visualizes temperature variations on the skin surface. Since inflammation generates heat through increased blood flow, metabolic activity, and immune response, thermography can highlight “hot spots” that may indicate underlying inflammatory processes, including in the pelvic region.
While not a standalone diagnostic tool for pelvic conditions, emerging research explores its use as a complementary method to identify physiological changes related to pelvic inflammation, chronic pelvic pain, pelvic floor dysfunction, and certain gynecological issues.
How Thermal Imaging Detects Inflammation
Infrared cameras capture the body’s emitted heat (infrared radiation) and convert it into color-coded images (thermograms). Warmer areas typically appear as red, orange, or white, while cooler areas show as blue or green.
- Inflammation principle: Inflamed tissues are “hotter” due to vasodilation and increased perfusion. Thermography measures relative temperature differences (often more reliable than absolute values) between symmetric body areas or compared to baseline.
- Procedure: The scan is painless, contact-free, and takes 15–30 minutes. Patients acclimate in a temperature-controlled room, and images are taken of the lower abdomen, pelvis, back, or perineum. No radiation, compression, or contrast is involved.
- Advantages: Quick, safe for repeated use (including during pregnancy in some contexts), and provides real-time physiological insights rather than just structural anatomy.
Potential Applications in Pelvic Inflammation Detection
Thermal imaging is primarily investigated for detecting or monitoring conditions involving heat-generating inflammation in the pelvic area:
- Pelvic Inflammatory Disease (PID) and related infections: Some studies note asymmetric or elevated temperatures in the lower abdomen associated with inflammatory processes, such as in high-risk HPV cervical infections or adnexal inflammation. Disrupted thermal patterns in the lower abdomen may reflect local inflammatory responses.
- Chronic Pelvic Pain and Pelvic Floor Dysfunction: Thermography has been used to evaluate female pelvic floor muscles. It can detect temperature changes at rest versus during contraction, showing correlations with muscle function measured by manometry. Warm colors may increase in the central pelvic area during contraction in healthy muscles. It may also help identify myofascial pain or functional impairments not visible on standard imaging.
- Endometriosis, PCOS, or menstrual-related issues: Practitioners in wellness settings sometimes use it to spot heightened heat patterns in the pelvic region that could suggest inflammation or vascular changes, though evidence is limited and not diagnostic.
- Postpartum or post-surgical inflammation: It can objectively track acute inflammatory changes, trauma-related swelling, or healing progress.
- Broader pelvic pain syndromes: Thermal asymmetry or hot spots may indicate nerve dysfunction, vascular issues, or musculoskeletal strain in the pelvic-femoral region.
It is also promoted in some clinics for general wellness screening to detect early inflammation before symptoms worsen.
Benefits of Thermal Imaging for Pelvic Concerns
- Non-invasive and patient-friendly: No pain, radiation, or internal exams required.
- Early physiological insights: May reveal inflammation or circulatory changes years before structural damage appears on ultrasound, MRI, or CT.
- Monitoring tool: Useful for tracking treatment response (e.g., after pelvic floor therapy, antibiotics, or anti-inflammatory interventions) by showing reductions in hot spots.
- Complementary to other modalities: Can provide functional data alongside anatomical imaging like ultrasound (first-line for PID) or MRI.
Limitations and Current Evidence
Thermal imaging is not a replacement for standard diagnostic methods:
- Limited specificity: Heat can result from many causes (inflammation, infection, muscle activity, circulation issues, or even external factors like clothing or room temperature). It does not identify the exact cause or provide detailed anatomy.
- Not validated as primary diagnostic: For conditions like PID, endometriosis, or pelvic organ issues, ultrasound, MRI, CT, and clinical exams (including labs) remain the gold standard. Thermography is considered adjunctive or experimental in pelvic applications.
- Evidence level: Most studies on pelvic thermography are small, preliminary, or focused on pelvic floor muscle evaluation rather than broad inflammation detection. Larger clinical trials are needed for routine use in gynecology or urology.
- Variability: Results depend on technician expertise, camera quality, patient preparation, and interpretation protocols. It performs better for relative (asymmetric) changes than absolute temperatures.
- Here’s a clear, balanced comparison between thermography (infrared thermography or thermal imaging) and ultrasound specifically in the context of pelvic inflammation detection, pelvic floor assessment, chronic pelvic pain, and related conditions like pelvic inflammatory disease (PID) or endometriosis.
Fundamental Difference in What They Measure
Thermography (Infrared Thermography – IRT): A functional/physiological imaging method. It detects and visualizes heat patterns and temperature differences on the skin surface caused by increased blood flow, inflammation, or metabolic activity. It does not show internal structures.
Ultrasound: A structural/anatomical imaging method. It uses high-frequency sound waves to create real-time images of organs, tissues, muscles, cysts, masses, fluid collections, and blood flow (via Doppler). It provides detailed internal anatomy.
In short: Thermography shows how the body is functioning (e.g., where inflammation is generating heat), while ultrasound shows what the body looks like inside (e.g., thickened tubes in PID or endometriomas).
Side-by-Side Comparison
Aspect
Thermography (IRT)
Ultrasound
Type of Information
Physiological (heat/inflammation, vascular activity)
Anatomical + functional (structure, size, blood flow)
Invasiveness
Completely non-contact, no probe on skin
Non-invasive; can be transabdominal (external) or transvaginal/transperineal (internal probe)
Radiation
None
None
Pain/Discomfort
None; very comfortable
Usually none, but internal probes can cause discomfort for some (especially with pelvic pain)
Time
15–30 minutes (full acclimation + scanning)
10–20 minutes
Best For Pelvic Inflammation
Detecting surface heat patterns suggesting inflammation, increased blood flow, or muscle activity
Visualizing internal signs of inflammation (e.g., fluid in fallopian tubes, ovarian swelling in PID, abscesses)
Pelvic Floor Assessment
Can show temperature/color changes during contraction vs rest; useful for overall muscle function in some studies
Real-time visualization of pelvic floor muscle movement, thickness, and coordination (especially transperineal ultrasound); widely used in pelvic floor physical therapy
Endometriosis/PID
May highlight hot spots or asymmetry related to inflammation; limited evidence; not diagnostic
First-line imaging for PID; good for detecting endometriomas and deep endometriosis when performed by experts; higher accuracy for structural changes
Early Detection
Potentially shows physiological changes before major structural damage
Excellent for structural abnormalities once present; less sensitive to very early subtle inflammation
Monitoring Treatment
Good for tracking reduction in inflammation/heat over time (e.g., after therapy or medication)
Excellent for monitoring structural changes, resolution of fluid, or muscle function
Limitations
Low specificity (heat can come from many causes); not validated as a primary diagnostic tool for pelvic conditions; operator and environmental dependent
Operator-dependent; limited view of superficial peritoneal endometriosis or adhesions; internal exam may not be suitable for everyone
Cost & Availability
Often available in wellness/integrative clinics; variable insurance coverage
Widely available, usually covered by insurance for medical indications
Strengths of Each in Pelvic Health Context
Thermography advantages:
Truly non-contact and highly comfortable — ideal for patients with severe pelvic pain, vaginismus, or those who cannot tolerate internal exams.
May detect early inflammatory or vascular changes.
Useful as a complementary monitoring tool (e.g., before/after pelvic floor therapy or anti-inflammatory treatment).
No risk of discomfort or infection from probes.
Ultrasound advantages:
Provides direct visualization of pelvic organs, making it the standard for diagnosing PID, ovarian cysts, fibroids, and many cases of endometriosis.
Real-time dynamic imaging — especially valuable in pelvic floor physical therapy to see muscle contractions and guide exercises.
Higher diagnostic accuracy for structural pelvic pathology when performed expertly.
When they complement each other: Many practitioners use thermography to identify areas of inflammation or asymmetry and then target ultrasound (or other imaging) for detailed structural evaluation. This “road map” approach can make ultrasound more focused and efficient.
Current Evidence and Recommendations
Ultrasound is well-established and recommended as a first-line imaging tool for pelvic inflammatory disease, suspected endometriosis (especially expert transvaginal or transperineal ultrasound), and pelvic floor dysfunction assessment.
Thermography remains largely adjunctive or experimental for pelvic applications. While promising for pelvic floor muscle evaluation and inflammation monitoring, it lacks large-scale validation as a standalone diagnostic for PID, endometriosis, or most pelvic conditions. It should not replace standard medical imaging or clinical evaluation.
Bottom Line for Patients
If you have symptoms of pelvic inflammation, pain, leakage, or suspected PID/endometriosis → start with a medical evaluation that may include ultrasound (often the most practical and informative first step).
If you’re looking for a completely non-contact way to monitor inflammation or pelvic floor function (e.g., in wellness settings or when internal exams are difficult), thermography can provide useful physiological insights as a supportive tool.
The best approach is often combined use under professional guidance rather than choosing one over the other.
Disclaimer: This information is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Imaging choices depend on your specific symptoms, history, and clinical needs. Always consult a qualified healthcare provider (such as a gynecologist, urogynecologist, or pelvic floor physical therapist) to determine the most appropriate tests for you. Do not rely on any single imaging modality in isolation for health decisions.
Would you like me to expand on any section, add a table for pelvic floor therapy specifically, or integrate this into your larger pelvic health article series?
It is generally not recommended as a sole method for diagnosing serious conditions like endometriosis or PID.
Who Might Consider Thermal Imaging?
It may appeal to individuals seeking non-invasive screening for:
- Unexplained chronic pelvic pain
- Suspected pelvic floor muscle issues (in conjunction with physical therapy assessment)
- Monitoring inflammation in wellness or integrative health settings
- Those who cannot tolerate radiation or invasive procedures
Always discuss with a healthcare provider. A pelvic floor specialist, gynecologist, or urogynecologist can determine if it adds value alongside conventional tests.
Disclaimer
This article is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Thermal imaging results must be interpreted by qualified practitioners and correlated with clinical findings. Consult your doctor before pursuing any imaging or wellness screening, especially if you have pelvic pain, suspected infection, pregnancy, or other symptoms. Do not rely on thermography alone for health decisions.
Thermal imaging offers an intriguing, safe window into the body’s inflammatory processes and pelvic floor function. While promising as a supportive tool, it works best as part of a comprehensive evaluation. If you’re experiencing pelvic symptoms, prioritize evidence-based care from a qualified specialist—early attention often leads to better outcomes.