❓ What is the most accurate test for oral cancer?
The most accurate test for oral cancer is a biopsy, where a tissue sample is examined under a microscope. However, newer methods like liquid biopsy and oral cancer biomarkers testing are improving early detection and monitoring.
❓ Are saliva tests reliable for detecting oral cancer?
Saliva tests for oral cancer are increasingly reliable for detecting early biomarkers like DNA, RNA, and proteins. While not a replacement for biopsy, they are a valuable non-invasive screening tool for early detection.
❓ Who should get tested for oral cancer biomarkers?
People at higher risk should consider oral cancer biomarker testing, including those who use tobacco or alcohol, have HPV infection, persistent mouth lesions, or are over age 30–40.
❓ Can oral cancer be detected before symptoms appear?
Yes, early detection oral cancer biomarkers can identify molecular changes before visible symptoms develop. This allows for earlier diagnosis and significantly improves treatment outcomes.
❓ What are the early warning signs of oral cancer?
Early signs include persistent mouth sores, red or white patches, lumps, difficulty swallowing, and unexplained pain. If symptoms last more than two weeks, a dental or medical evaluation is recommended.
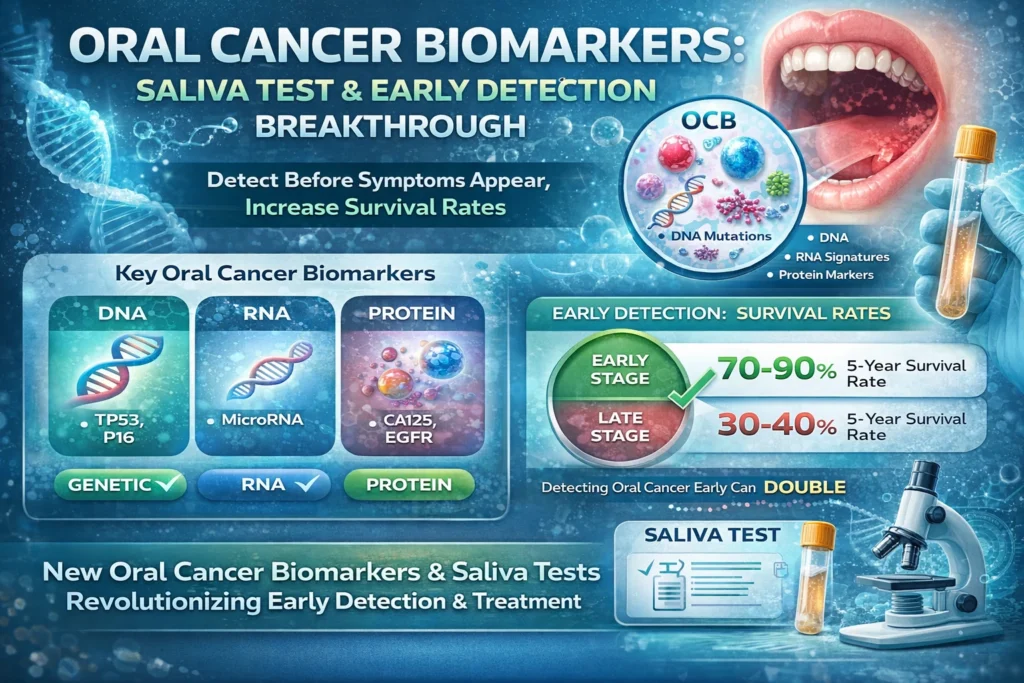
Every hour of every day, someone in the United States dies from oral cancer. According to the Oral Cancer Foundation, approximately 54,000 Americans will be diagnosed with oral or oropharyngeal cancer this year. While these statistics are sobering, they come with a critical caveat: when detected early, the survival rate for oral cancer is nearly 90%.
The problem lies not in treatment, but in timing. Historically, detection has relied on visual examination—a dentist or doctor looking for suspicious red or white patches, lumps, or sores. By the time these physical symptoms are visible, the disease is often already in its later stages (III or IV).

But the landscape of oncology is shifting. We are entering an era where a simple, painless saliva test could replace the anxiety of the “watch and wait” approach. Central to this revolution are oral cancer biomarkers—biological clues hiding in plain sight. For patients and healthcare providers in the USA, understanding these tools is the key to changing the prognosis of this disease.
The Silent Epidemic: Why Early Detection Matters
Oral cancer is often called a “silent killer.” In its early stages, it frequently presents no pain. Patients might ignore a small ulcer, assuming it’s a canker sore, or dismiss a persistent sore throat as allergies. By the time a lump is palpable in the neck or swallowing becomes difficult, the cancer has often metastasized.
The traditional screening method—visual and tactile examination—is subjective. It relies heavily on the expertise of the clinician. While dentists are the unsung heroes in this fight (they are often the first line of defense), they are human. Studies show that visual screening alone can miss up to 25% of early-stage lesions.
This gap in diagnostic accuracy has created an urgent need for objective, molecular-level diagnostics. This is where the science of biomarkers comes into play.
Unlocking the Code: What Are Oral Cancer Biomarkers?
To understand the future of screening, we must first understand the language of cancer. Oral cancer biomarkers are measurable indicators of biological processes. They are the “molecular fingerprints” left behind by malignant cells.
These biomarkers can be found in tissue (biopsies), blood, or—most promisingly—saliva. They come in various forms:
- Genomic Biomarkers (DNA/RNA): Cancer cells often have mutated DNA or overexpress certain genes. For instance, mutations in the TP53 tumor suppressor gene are found in a significant percentage of oral cancers. Similarly, microRNAs (miRNAs)—tiny pieces of non-coding RNA that regulate gene expression—are often dysregulated in cancer patients.
- Proteomic Biomarkers (Proteins): Cancer cells produce specific proteins, such as cytokines (like IL-8) and growth factors. Elevated levels of these proteins in saliva can indicate the presence of malignancy.
- Transcriptomic Biomarkers (mRNA): Messenger RNA (mRNA) levels can show which genes are actively being “read” to produce proteins. Certain mRNA sequences, such as SAT and *IL-8*, have been validated as high-accuracy biomarkers for oral squamous cell carcinoma (OSCC), the most common form of oral cancer.
The beauty of these biomarkers is that they are shed directly into the oral cavity by the tumor itself. Unlike a blood test, which requires a needle and often shows systemic (body-wide) inflammation, saliva offers a “proximal fluid”—a direct sample of the environment where the cancer is brewing.
The Game Changer: The Saliva Test for Oral Cancer
Imagine walking into your dentist’s office for a routine cleaning. Instead of just a visual exam, you are asked to rinse your mouth with a solution and spit into a vial. A week later, your dentist knows not just if you have cavities, but if you have the molecular signature of early-stage cancer.
This is the promise of the saliva test for oral cancer. For years, this concept was science fiction. Today, it is a clinical reality gaining traction across the USA.
🧪 Types of Oral Cancer Biomarkers
🧬 Genetic Biomarkers
- Detect mutations in cancer-related genes
- Used for risk prediction and targeted therapy
🧪 Protein Biomarkers
- Reflect tumor activity and inflammation
- Help monitor disease progression
💧 Salivary Biomarkers
- Found in saliva (DNA, RNA, proteins)
- Best for non-invasive screening
🩸 Blood-Based Biomarkers (Liquid Biopsy)
- Circulating tumor DNA (ctDNA)
- Used for real-time monitoring and recurrence detection
How It Works
Modern saliva tests utilize technologies like liquid biopsy. Unlike a surgical biopsy, which removes a piece of tissue, a liquid biopsy captures tumor-derived material from bodily fluids.
In the context of a saliva test:
- Collection: A patient provides a small sample of saliva (usually 1-2 mL).
- Stabilization: The sample is mixed with a stabilizing solution to preserve the RNA, DNA, and proteins for up to several days.
- Analysis: Using advanced techniques like Polymerase Chain Reaction (PCR) or Next-Generation Sequencing (NGS), labs scan the sample for the specific oral cancer biomarkers mentioned earlier.
- Risk Stratification: The software analyzes the concentration of these biomarkers. If the “signature” matches that of malignancy, the patient is flagged for immediate follow-up, typically a gold-standard scalpel biopsy for histopathological confirmation.
- How Biomarkers Improve Early Detection
Traditional detection relies on:
Visual exam
Biopsy
👉 Biomarkers go further by:
Identifying microscopic disease changes
Detecting cancer before symptoms
Enabling routine screening in dental clinics
💉 Management of Oral Cancer Using Biomarkers
Biomarkers are transforming how oral cancer is treated:
✔️ Personalized Treatment
Match therapies based on biomarker profile
Example: targeting EGFR pathways
✔️ Monitoring Treatment Response
Track biomarker levels during therapy
Adjust treatment if needed
✔️ Detecting Recurrence Early
Liquid biopsy and saliva tests help identify relapse sooner
Future of Oral Cancer Detection in the U.S.
The next wave includes:
- At-home saliva testing kits
- AI-integrated diagnostic platforms
- Real-time cancer monitoring apps
- Personalized treatment plans based on biomarker profiles
👉 The goal is clear:
Detect oral cancer before symptoms appear
🎯 Why This Matters for U.S. Patients
Early detection can:
- Increase survival rates significantly
- Reduce need for aggressive treatments
- Lower healthcare costs
👉 Biomarkers are shifting care from:
Late-stage treatment → Early prevention and precision medicine
Leading the Charge: Innovations in the USA
The United States is currently a hub for this diagnostic innovation. Several academic institutions and biotech companies are leading the way.
For instance, research emanating from the University of California, Los Angeles (UCLA) School of Dentistry has been pivotal. Dr. David Wong and his team have spent decades developing technologies like the “Electric Field-Induced Release and Measurement” (EFIRM) platform, which can detect cancer-related biomarkers in saliva with high sensitivity.
In 2024 and 2025, we are seeing a shift from research labs to commercial availability. Companies are now offering FDA-approved (or in-process) saliva-based tests designed to act as adjuncts to the visual exam. These tests are not meant to replace the biopsy, but rather to act as a triage tool, helping clinicians decide which patients need a biopsy and which can be safely monitored.
Early Detection: The Ultimate Goal
The synergy of oral cancer biomarkers and the saliva test for oral cancer creates a powerful framework for early detection oral cancer biomarkers.
Why is early detection so critical?
- Morbidity: Late-stage oral cancer often requires aggressive treatment: radical neck dissection, radiation, and chemotherapy. This can lead to severe disfigurement, difficulty speaking, and chronic dry mouth. Early-stage treatment is often less invasive and preserves quality of life.
- Mortality: As mentioned, the survival rate plummets from 90% (Stage I) to under 40% (Stage IV) once the cancer spreads to distant sites.
- Cost: The cost of treating late-stage cancer is astronomically higher than treating early-stage disease, both for the patient and the healthcare system.
By utilizing early detection oral cancer biomarkers, we can identify patients with “field cancerization”—areas of the mouth that appear normal but are genetically primed to become cancerous—years before a tumor physically forms.
Who Should Be Tested?
While the general population is at risk, certain demographics in the USA have a significantly higher risk profile. The ideal candidates for adjunctive saliva testing include:
- Traditional Risk Users: Those who use tobacco (smoking, chewing, vaping) and heavy alcohol users. This demographic has historically accounted for the majority of oral cancer cases.
- HPV-Positive Individuals: Over the last two decades, the face of oral cancer has changed. The Human Papillomavirus (HPV), specifically HPV-16, is now the leading cause of oropharyngeal cancers (back of the throat, tonsils) in the USA. These cancers are rising rapidly in young, non-smoking adults. Biomarker tests can differentiate between HPV-positive and HPV-negative tumors, which often have different prognoses.
- History of Oral Cancer: Patients who have had oral cancer before are at a higher risk of recurrence or developing a second primary cancer.
- The “Worried Well”: Patients with persistent symptoms that don’t have an obvious visual cause—such as a chronic sore throat, ear pain without infection, or a feeling of something stuck in the throat—can benefit from the objective data a saliva test provides.
- 📊 Survival Benefits of Biomarker-Based Detection
Stage of Detection
5-Year Survival Rate
Early stage
70–90%
Advanced stage
30–40%
👉 Early detection using oral cancer biomarkers can double survival chances - Risk Factors (USA Context)
Tobacco use (smoking, chewing)
Alcohol consumption
HPV infection
Poor oral hygiene
👉 High-risk individuals benefit most from saliva test for oral cancer screening
🏥 Role of Dentists in Early Detection
In the U.S., dentists are key to prevention:
Routine oral exams
Use of salivary biomarker tests
Referral for further evaluation
👉 Dental visits are becoming first-line cancer screening opportunities - 🧠 Bottom Line
- Oral cancer biomarkers are revolutionizing cancer care:
- 🔍 Enable early detection
- 💧 Power saliva test for oral cancer
- 🎯 Improve treatment precision
- 📈 Increase survival rates significantly
- 👉 The shift is clear:
- From late diagnosis → early detection → better survival
Challenges and Considerations
Despite the immense promise, the integration of salivary diagnostics into mainstream dentistry and medicine in the USA faces hurdles.
- Insurance Reimbursement: Currently, many saliva-based cancer tests are considered “emerging technology.” While some dental and medical insurance plans are beginning to cover them, others require out-of-pocket payment. As the evidence base solidifies, we expect coding and reimbursement to catch up.
- False Positives/Negatives: No test is perfect. A positive saliva test requires a scalpel biopsy to confirm. Conversely, a negative test does not guarantee a clean bill of health if clinical suspicion remains high. These tests are best used as adjunctive tools, not standalone diagnostic solutions.
- Education: There is a knowledge gap among general dentists and primary care physicians. Many clinicians are not yet aware that these tests exist or how to integrate them into their workflow. Patient advocacy will likely drive adoption as awareness grows.
The Future of Oral Cancer Diagnostics
Looking ahead, the future of early detection oral cancer biomarkers is trending toward personalization and accessibility.
We are moving toward Point-of-Care (POC) devices. Imagine a handheld device in a dental office that can process a saliva sample in 15 minutes, providing a “yes/no” risk assessment before the patient even leaves the chair. This would eliminate the logistical hurdle of sending samples to central labs.
Furthermore, researchers are developing multi-analyte panels. Instead of looking for just one protein or one gene, future tests will analyze a panel of hundreds of biomarkers simultaneously. Using artificial intelligence (AI), these tests will be able to identify complex patterns that the human eye cannot see, drastically improving accuracy.
Conclusion: A Call to Action
The narrative around oral cancer is changing. For decades, the medical community has relied on the same visual inspection techniques used by our predecessors. While dental professionals do an admirable job, we have reached the limits of what the naked eye can achieve.
The convergence of oral cancer biomarkers USA research, the clinical availability of the saliva test for oral cancer, and the relentless pursuit of early detection oral cancer biomarkers offers the most significant leap forward in a generation.
If you are a patient in the USA, particularly if you have risk factors like HPV, tobacco use, or a family history of cancer, ask your dentist or primary care provider: “Do you offer salivary biomarker testing?” If you are a healthcare provider, now is the time to explore integrating these molecular diagnostics into your practice.
We stand on the brink of making oral cancer a largely preventable and highly treatable disease. The tools are no longer in the future—they are here, in the present, flowing in the most accessible fluid our bodies produce. It’s time we started listening to what our saliva is trying to tell us.
Faqs :
❓ What are oral cancer biomarkers and why are they important?
Oral cancer biomarkers are biological molecules found in blood, saliva, or tissues that indicate the presence of cancer. They are important because they enable early detection, risk assessment, and personalized treatment, significantly improving survival rates.
❓ How does a saliva test for oral cancer work?
A saliva test for oral cancer analyzes saliva for DNA, RNA, and protein biomarkers linked to cancer. It is a non-invasive, quick, and cost-effective method that can detect early-stage oral cancer during routine dental visits.
❓ Can early detection oral cancer biomarkers improve survival rates?
Yes, early detection oral cancer biomarkers can dramatically improve outcomes. When oral cancer is detected early, the 5-year survival rate can reach 70–90%, compared to much lower rates in advanced stages.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment options regarding oral health or cancer.