By Dr. mohammed abdul azeem siddiqui
Reviewed for emerging diagnostic trends in women’s health
Let’s be honest: most women hate Pap smears. The speculum. The scraping. The anxiety while waiting for results.
But what if you could detect early cervical disease — including HPV-related changes and inflammation — using nothing more than your body’s own cervical mucus?
It sounds futuristic. But researchers at Johns Hopkins and the University of Washington are now calling cervical mucus a “liquid biopsy” for the cervix. And the best part? It’s non-invasive, painless, and potentially doable at home.
So, is cervical mucus the next breakthrough in early cervical cancer detection? Let’s dive into the science.
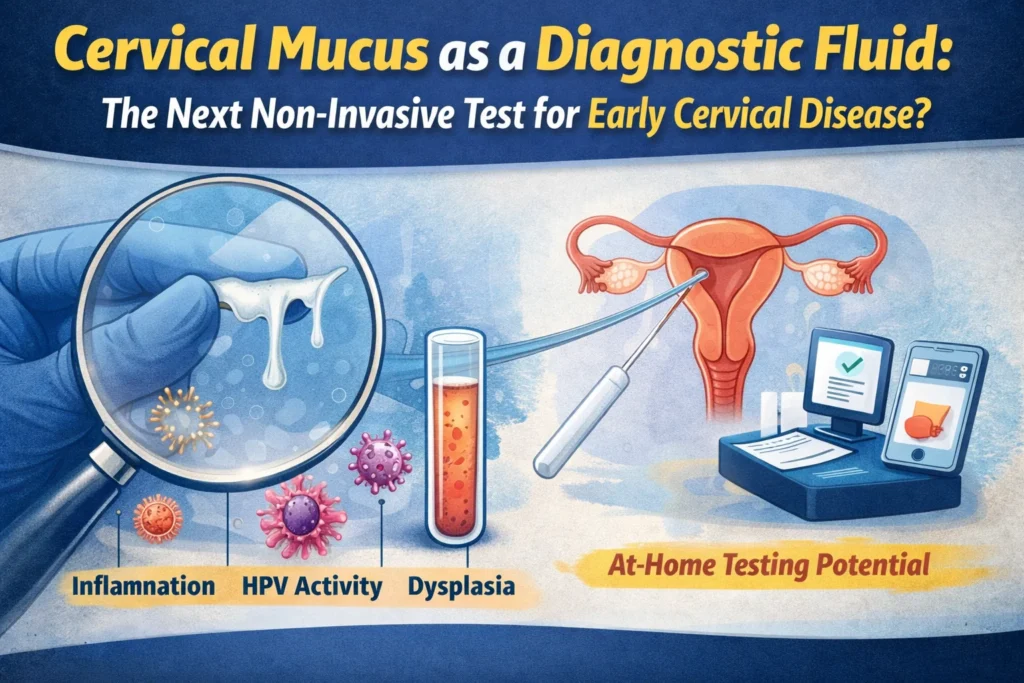
What Makes Cervical Mucus a Diagnostic Goldmine?
Cervical mucus isn’t just for tracking ovulation. It is a dynamic biological fluid produced by the cervical crypts. It contains:
- Exfoliated cervical cells (same ones a Pap smear collects).
- Viral DNA (including high-risk HPV strains).
- Inflammatory cytokines (markers of chronic inflammation).
- Proteins and metabolites that change when cells turn cancerous.
In simple terms: your mucus is a mirror of your cervical health. Every day, your cervix sheds cells and secretions into the mucus. Collecting that fluid is like taking a biopsy without a needle or speculum.
“Cervical mucus is an underutilized diagnostic reservoir,” says Dr. Rebecca Brotman, a leading vaginal microbiome researcher. “It tells us about infection, inflammation, and even precancerous changes.”
The Problem with Current Testing (And Why Mucus Wins)
| Test | Invasive? | Pain? | At-Home? | Cost (USA) |
|---|---|---|---|---|
| Pap Smear | Yes | Mild to moderate | No | $50–$200+ |
| Colposcopy/Biopsy | Yes | Moderate to high | No | $300–$1,000+ |
| HPV DNA Test | Yes (swab) | Mild | Rarely | $75–$150 |
| Cervical Mucus Test | No | None | Yes | $15–$50 (estimated) |
A Pap smear requires a healthcare provider to scrape cells directly from the cervix. But cervical mucus flows out naturally every day. You can collect it yourself with a simple swab or even a menstrual cup.
That’s why major diagnostic companies (including Roche and Hologic) are now investing in self-collected vaginal and cervical mucus tests.
What Can Cervical Mucus Detect Right Now?
While the FDA hasn’t fully approved a stand-alone “mucus cancer test” yet, researchers have already proven it can detect:
1. High-Risk HPV DNA
Several studies show that HPV DNA detected in self-collected cervical mucus matches 94–98% of clinician-collected samples. That means you could swab at home and mail it to a lab.
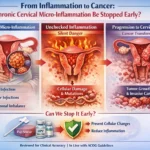
2. Inflammatory Markers (IL-6, TNF-alpha, CRP)
Chronic inflammation is the bridge between HPV infection and cancer. Mucus levels of these cytokines rise years before abnormal cells appear.
3. Abnormal Glycoproteins (MUC16, CA-125)
Cancer cells change the sugar coating of mucus. These altered proteins can be detected in fluid samples long before a Pap smear turns abnormal.
4. Microbiome Imbalances
Certain bacteria (Fusobacterium, Sneathia) are linked to cervical precancer. Mucus tells you exactly which bacteria are present.
How You Can Start Using Cervical Mucus for Early Detection Today (Even Without a Prescription)
While you wait for FDA-approved mucus cancer tests, you can already use cervical mucus to monitor inflammation and infection risk at home. Here’s how.
Step 1: Collect Your Mucus Properly
You don’t need a doctor. Use one of these methods:
- Clean finger insertion (wash hands first).
- Sterile swab (insert 1–2 inches, rotate gently).
- Menstrual cup (wear for 1–2 hours during non-menstrual days).
Pro tip: Collect in the morning before urinating or bathing for the most concentrated sample.
Recommended Collection Tools on Amazon
- Pre-sterilized vaginal swabs – perfect for home collection.
👉 Buy Sterile Vaginal Swabs on Amazon - Sacky 2-Pack Menstrual Cup – great for mucus collection (use it on non-period days).
👉 Shop Menstrual Cup on Amazon
Step 2: Test Your Mucus pH at Home
Cancerous and inflamed cervical mucus becomes less acidic (pH rises above 4.5). This is one of the earliest warning signs.
- Normal healthy cervical mucus pH: 3.8 – 4.5
- Inflamed or dysplastic mucus pH: 5.0 – 7.0
Best-Selling pH Test Kit on Amazon
- Natureland Vaginal pH Test Strips (FDA registered, 50 tests per box).
👉 Check pH Strips on Amazon
How to use:
Collect mucus on a swab → wipe onto the test strip → compare color within 30 seconds.
If your pH is consistently above 5.0, see a gynecologist and ask for a colposcopy.
Step 3: Look for Visible Abnormalities
Healthy cervical mucus is:
- Clear or white.
- Stretchy (like egg whites) mid-cycle.
- Odorless or mildly tangy.
Warning signs in mucus (see a doctor):
- Yellow, green, or brown tinge.
- Thick, clumpy, or cottage-cheese texture (yeast).
- Fishy odor (bacterial vaginosis).
- Blood-tinged mucus outside of your period.
Note: Blood in cervical mucus between periods is called post-coital or intermenstrual bleeding. It is a red flag for cervical inflammation or dysplasia.
Step 4: Support Healthy Cervical Mucus (Anti-Inflammatory Protocol)
Healthy mucus = healthy cervix. You can improve your mucus quality and reduce inflammation with these supplements.
A. N-Acetylcysteine (NAC)
NAC breaks down thick, inflammatory mucus and has been shown to reverse HPV-related cervical dysplasia in some studies.
- Best on Amazon: NOW Foods NAC 600 mg (vegan, USA-made).
👉 Buy NAC on Amazon
B. Vaginal Probiotics (Lactobacillus crispatus)
Healthy mucus is acidic and rich in good bacteria. Probiotics restore that balance.
- Top USA Pick: Physician’s Choice Vaginal Probiotic (60 Billion CFU + prebiotic).
👉 Get Vaginal Probiotics on Amazon
C. DIM + Broccoli Sprout Extract
These compounds help your liver clear out inflammatory estrogens and activate anti-cancer pathways in cervical tissue.
- Best DIM Supplement: Nutricost DIM 300 mg + BioPerine.
👉 Shop DIM on Amazon
What’s Coming in the Next 2–5 Years?
Several biotech startups are racing to bring at-home cervical mucus diagnostic kits to the US market. Here’s what’s in the pipeline:
| Product | What It Detects | Estimated Launch |
|---|---|---|
| Teal Health’s At-Home HPV Test | High-risk HPV (self-swab) | Late 2025 |
| Juniper Diagnostics | Inflammatory cytokines + HPV | 2026 |
| MucusCheck (prototype) | MUC16 + CA-125 proteins | 2027 |
Until then, the best strategy is to combine at-home mucus monitoring (pH + visual checks) with annual Pap smears.
When to See a Doctor (Don’t Rely Only on Mucus)
At-home mucus testing is complementary, not a replacement. See a gynecologist immediately if you have:
- Any post-coital bleeding (blood after sex).
- Persistent pelvic pain not linked to your period.
- Mucus pH above 5.5 for two consecutive weeks.
- Blood-tinged mucus without a known cause.
Ask your OB/GYN for a self-collected HPV test if they offer it. Many clinics now allow you to swab yourself in the exam room.
The Bottom Line for American Women
Cervical mucus is no longer just “that discharge you ignore.” It is a powerful diagnostic fluid that can reveal inflammation, HPV, and even early cancer signs — without a single invasive scrape.
While the FDA hasn’t fully approved home mucus cancer tests yet, you can start today by:
- Collecting mucus with sterile swabs or a menstrual cup.
- Testing pH weekly with affordable strips.
- Supporting mucus health with NAC, probiotics, and DIM.
- Tracking changes and sharing them with your doctor.
The future of cervical screening is non-invasive, painless, and in your hands. Literally.
Ready to Start Monitoring Your Cervical Mucus at Home?
Build your DIY cervical mucus diagnostic kit on Amazon:
- Sterile vaginal swabs (for clean collection)
- Vaginal pH test strips (for early warning)
- NAC + probiotics + DIM (for cervical health)
👉 Click Here to Shop the Complete Cervical Mucus Monitoring Kit
Disclaimer: This article contains affiliate links. As an Amazon Associate, I earn from qualifying purchases. This information is for educational purposes only and is not a substitute for professional medical advice. Always consult your gynecologist before changing your health regimen, especially if you have a history of abnormal Pap smears, HPV, or cervical dysplasia.