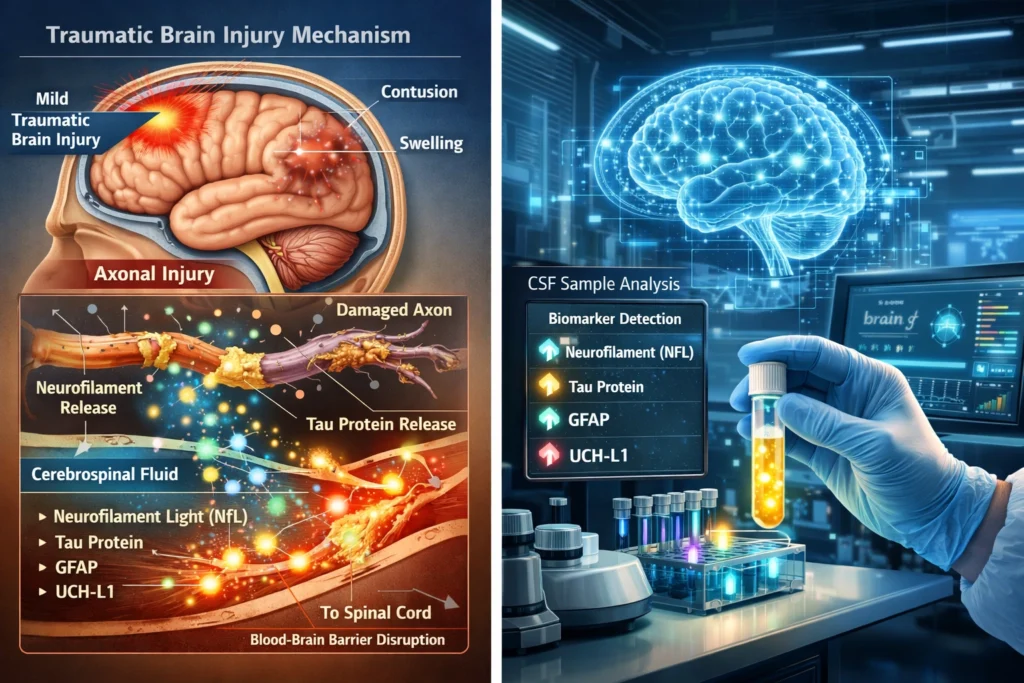
Brain injuries are often associated with dramatic events—car accidents, severe falls, or sports collisions. However, not all brain injuries produce immediate symptoms. In many cases, repeated mild head impacts cause microscopic neuronal damage that goes unnoticed for years.
This phenomenon is known as silent neurotrauma. Individuals may appear perfectly healthy while subtle damage accumulates within the brain. Over time, this hidden injury may contribute to cognitive decline, memory problems, and neurodegenerative diseases.
Scientists are now discovering that cerebrospinal fluid (CSF) biomarkers may reveal these hidden injuries long before traditional brain scans detect abnormalities.
Research in neuroscience and neurology is increasingly focusing on CSF proteins released during neuronal injury, offering a promising new method for detecting Traumatic Brain Injury (TBI) at very early stages.
What Is Silent Neurotrauma?
Silent neurotrauma refers to subclinical brain injury caused by repetitive mild head trauma that does not immediately produce symptoms such as loss of consciousness or severe neurological deficits.
Common situations where silent neurotrauma occurs include:
- contact sports such as football, boxing, and hockey
- military blast exposure
- repeated minor accidents
- occupational head impacts
Although each impact may seem insignificant, cumulative damage can disrupt neuronal networks over time.
Researchers believe silent neurotrauma may increase the risk of long-term neurological conditions such as:
- Chronic Traumatic Encephalopathy
- Alzheimer’s disease
- cognitive impairment and memory decline
Detecting these injuries early has become a major challenge in neurology.
Why Traditional Brain Scans Often Miss Mild Brain Injury
Conventional diagnostic tools include:
- CT scans
- MRI scans
- neurological examinations
While these tools are effective for detecting major brain injuries, they often fail to identify microscopic neuronal damage caused by mild trauma.
Small changes such as:
- axonal stretching
- synaptic injury
- glial activation
may not be visible on imaging.
As a result, researchers are increasingly turning to biochemical biomarkers in cerebrospinal fluid.
What Are CSF Biomarkers?
Cerebrospinal fluid surrounds the brain and spinal cord, acting as both a protective cushion and a transport system for nutrients and metabolic waste.
When brain cells are damaged, certain proteins are released into CSF. Measuring these proteins allows researchers to detect injury at a molecular level.
CSF biomarker analysis offers several advantages:
- extremely sensitive detection of neuronal damage
- early identification of injury before imaging changes
- monitoring of injury progression
- evaluation of treatment response
Key CSF Biomarkers of Silent Neurotrauma
Neurofilament Light Chain (NfL)
Neurofilament light chain is one of the most sensitive indicators of axonal injury.
Neurofilaments are structural proteins that maintain the stability of neuronal axons. When axons are damaged due to trauma, fragments of these proteins enter the CSF.
Elevated NfL levels have been observed in:
- athletes with repeated concussions
- patients with mild traumatic brain injury
- military personnel exposed to blast injuries
Studies show that higher NfL levels often correlate with the severity of neuronal damage.
Tau Protein
Tau protein stabilizes microtubules within neurons. When brain cells are injured, tau is released into the surrounding cerebrospinal fluid.
Two major forms are measured:
- total tau
- phosphorylated tau
Elevated tau levels are associated with:
- concussion
- axonal injury
- neurodegenerative processes
Abnormal tau accumulation is also a hallmark of Alzheimer’s disease and Chronic Traumatic Encephalopathy.
Glial Fibrillary Acidic Protein (GFAP)
GFAP is a protein found in astrocytes, a type of glial cell that supports neurons.
When brain injury occurs, astrocytes become activated and release GFAP into CSF and blood.
GFAP is particularly useful because it:
- indicates astrocyte injury
- helps distinguish brain trauma from non-neurological injuries
- rises quickly after traumatic brain injury
UCH-L1 (Ubiquitin C-Terminal Hydrolase L1)
UCH-L1 is a neuronal enzyme involved in protein degradation and cellular repair.
Following brain trauma:
- neurons release UCH-L1 into CSF and blood.
It is considered an early biomarker of neuronal cell body injury.
S100B Protein
S100B is another astrocytic protein released during brain injury.
Although it is less specific than other biomarkers, it remains useful for:
- detecting mild brain injury
- screening concussion patients
- identifying blood-brain barrier disruption
Why Silent Neurotrauma Is a Growing Concern
In recent years, researchers have become increasingly concerned about the long-term effects of repeated mild head injuries.
Studies involving athletes and military personnel suggest that cumulative brain trauma may lead to progressive neurological damage.
In particular, repetitive injury has been linked to Chronic Traumatic Encephalopathy, a degenerative brain disease associated with memory loss, behavioral changes, and cognitive decline.
Early detection of silent neurotrauma could help prevent these long-term consequences.
Clinical Applications of CSF Biomarkers
Early Diagnosis of Brain Injury
Biomarkers can detect neuronal damage even when imaging appears normal.
This allows clinicians to identify patients who may require rest and neurological monitoring.
Monitoring Recovery After Concussion
CSF biomarkers may help physicians determine when the brain has fully recovered from injury.
This is particularly important for athletes deciding when it is safe to return to play.
Risk Prediction for Neurodegenerative Disease
Persistent biomarker elevation may indicate increased risk for future neurological disorders.
Early detection allows doctors to monitor patients more closely and implement preventive strategies.
Drug Development and Clinical Trials
Pharmaceutical researchers are increasingly using CSF biomarkers as objective measures of brain injury and treatment response.
These biomarkers may accelerate the development of therapies designed to protect neurons after trauma.
The Future of Brain Injury Diagnostics
Rapid advances in neuroscience technology are expanding the possibilities of biomarker research.
Emerging areas include:
- microRNA biomarkers
- extracellular vesicle markers
- mitochondrial stress indicators
- synaptic protein fragments
Artificial intelligence may soon combine multiple biomarkers into predictive algorithms capable of estimating cumulative brain damage.
Such technologies could revolutionize the diagnosis and management of Traumatic Brain Injury.
Conclusion
Silent neurotrauma represents an important but often overlooked medical problem. Repeated mild head injuries can gradually damage neurons without producing immediate symptoms.
Cerebrospinal fluid biomarkers offer a powerful new tool for detecting these hidden injuries. Proteins such as neurofilament light chain, tau, GFAP, UCH-L1, and S100B provide valuable insight into neuronal and glial damage at a molecular level.
As research continues, CSF biomarker testing may become a routine method for identifying early brain injury, protecting vulnerable individuals, and preventing long-term neurological disease.
Understanding these hidden signals from the brain may ultimately transform how clinicians diagnose and treat Traumatic Brain Injury worldwide.