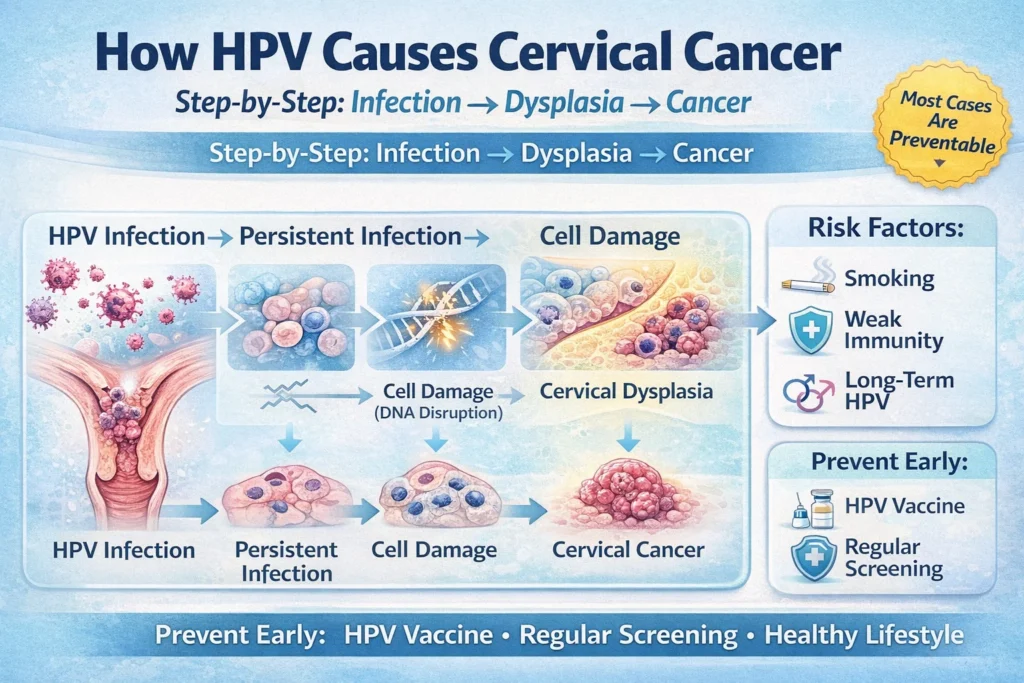
Cervical cancer remains one of the most preventable yet prevalent gynecological cancers worldwide, with human papillomavirus (HPV) responsible for nearly all cases. Understanding how HPV causes cervical cancer is crucial for early detection, prevention, and informed health decisions. This comprehensive, step-by-step guide breaks down the biological process, highlights risk factors for cervical dysplasia, explores chronic inflammation and cervical disease, and examines hormonal influence on cervical health.
Whether you’re researching symptoms, prevention strategies, or treatment options, this article provides clear, evidence-based insights. For expert consultations on women’s health and related concerns ,explore services .
What Is HPV and Why Does It Matter?
HPV is a common group of viruses transmitted primarily through skin-to-skin contact during sexual activity. Over 200 types exist, but high-risk HPV strains (especially HPV 16 and 18) are the primary culprits behind cervical cancer. Most HPV infections clear naturally within 1–2 years via the immune system, but persistent infections can lead to cellular changes over 10–20 years.
Early screening and HPV vaccination can prevent up to 90% of cases. If you’re concerned about HPV-related risks, professional evaluation at clinic,can provide personalized guidance.
Step-by-Step: How HPV Causes Cervical Cancer
Step 1: Transmission and Initial Infection
HPV enters the body through microscopic tears in the cervical lining during vaginal, anal, or oral sex. The virus targets basal epithelial cells in the cervix. Low-risk types cause warts, but high-risk types integrate silently without immediate symptoms.
Persistent Infection (The Critical Turning Point)
In most people (over 90%), the immune system clears HPV within 2 years. However, in 10% of cases, the infection persists due to factors like weakened immunity or repeated exposure. Persistent high-risk HPV is the key driver of progression.
Pro tip: Regular Pap smears and HPV DNA tests detect issues early. Schedule screenings .
Viral DNA Integration into Host Cells
The HPV genome integrates into the host cell’s DNA, disrupting the viral E2 gene (a regulator). This leads to uncontrolled production of oncoproteins E6 and E7.
Oncoprotein Action – Disrupting Tumor Suppressors
- E6 protein binds and degrades p53 (the “guardian of the genome”), preventing DNA repair and apoptosis (programmed cell death).
- E7 protein inactivates pRb, releasing E2F transcription factors that force cells into uncontrolled proliferation.
This duo creates genomic instability, allowing mutations to accumulate.
Cervical Dysplasia Develops
Abnormal cell growth results in cervical intraepithelial neoplasia (CIN), graded as CIN1 (mild), CIN2 (moderate), or CIN3 (severe). These precancerous lesions are detectable via biopsy but often asymptomatic.
Risk Factors for Cervical Dysplasia Several factors increase the likelihood of dysplasia in HPV-positive individuals:
- Smoking (doubles risk by impairing immune response and promoting inflammation).
- Weakened immune system (e.g., HIV, immunosuppressive drugs).
- Early sexual debut or multiple partners (higher HPV exposure).
- Long-term oral contraceptive use or multiple full-term pregnancies.
- Co-infections with other STIs (chlamydia, herpes).
Early intervention is key. Consult for risk assessment and preventive strategies.
Progression to Invasive Cervical Cancer
Untreated CIN3 can invade deeper cervical tissues, becoming squamous cell carcinoma (most common) or adenocarcinoma. This process takes 10–20 years in immunocompetent individuals but accelerates with HIV or chronic inflammation.
Chronic Inflammation and Cervical Disease
Chronic inflammation plays a pivotal role in HPV-driven cervical disease. Persistent HPV triggers ongoing immune activation, releasing cytokines and reactive oxygen species that damage DNA and promote cell survival. Studies link cervical inflammation (cervicitis) to higher-grade lesions in HPV-infected women.
Inflammation creates a tumor-friendly microenvironment, accelerating progression from dysplasia to cancer. Factors like smoking, untreated STIs, or autoimmune conditions exacerbate this. Managing inflammation through lifestyle changes and medical follow-up is essential. For comprehensive women’s health support addressing inflammation-related concerns.
Hormonal Influence on Cervical Health
Hormones significantly modulate cervical vulnerability to HPV.
- Oral contraceptives: Long-term use (>5–10 years) may increase risk by altering cervical mucus and cell turnover, though benefits (e.g., reduced ovarian/uterine cancer) often outweigh this in screened populations.
- Pregnancy and parity: Multiple full-term pregnancies elevate estrogen/progesterone exposure, potentially enhancing HPV persistence and E6/E7 expression.
- Estrogen signaling: Estrogen receptors (including GPR30) in cervical cells can amplify genomic instability in HPV-infected tissue, promoting proliferation and DNA damage.
Hormonal factors do not cause cancer independently but interact with persistent HPV. Balancing hormones and regular monitoring are vital. Discuss personalized hormonal health plans with experts .
Prevention and Early Detection: Your Best Defense
- HPV vaccination: Gardasil or Cervarix prevents high-risk strains (ideally before sexual activity).
- Regular screening: Pap tests + HPV co-testing starting at age 21–25.
- Lifestyle: Quit smoking, practice safe sex, maintain immunity.
- Treatment: For dysplasia, options include LEEP, cryotherapy, or monitoring.
Virtually all cervical cancers are preventable with vaccination and screening.
Conclusion: Take Control of Your Cervical Health
How HPV causes cervical cancer follows a clear, preventable pathway—from infection to persistent viral activity, cellular disruption, and eventual invasion. By understanding risk factors for cervical dysplasia, the role of chronic inflammation and cervical disease, and hormonal influence on cervical health, you empower yourself with knowledge.
Don’t wait for symptoms. Prioritize screening and expert care. For advanced consultations, treatments, and holistic women’s health services.. Early action saves lives—schedule your appointment and stay protected.
This article is for informational purposes only and not a substitute for professional medical advice. Always consult a qualified healthcare provider.