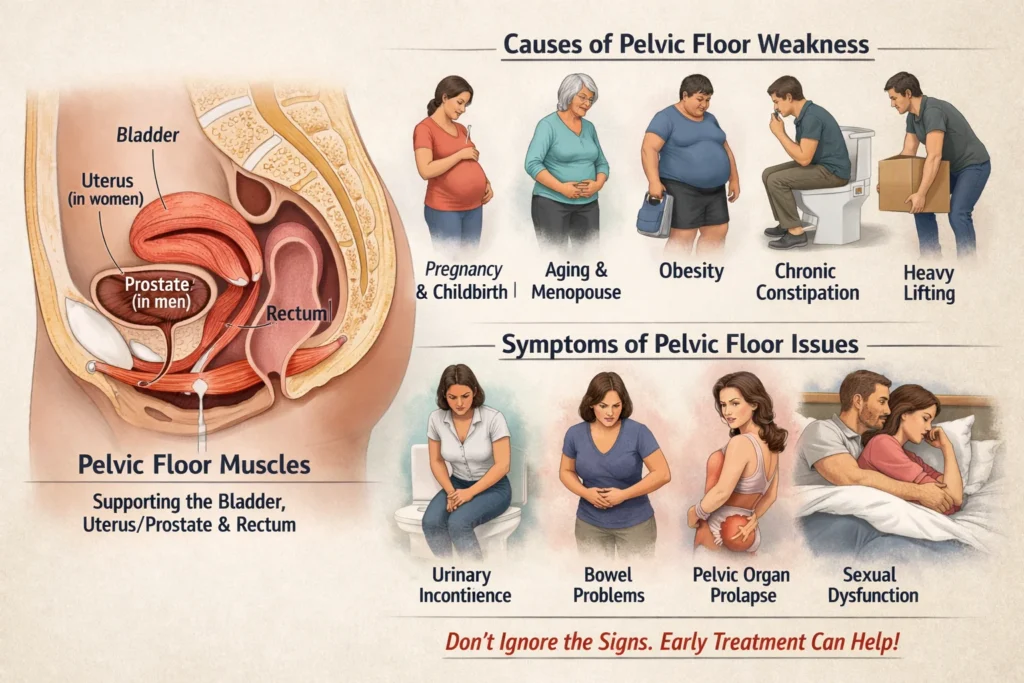
Pelvic floor muscles form a strong, hammock-like structure at the base of your pelvis, supporting the bladder, uterus (in women), prostate (in men), and rectum. They play a crucial role in controlling urination, bowel movements, sexual function, and core stability. But when these muscles weaken—often gradually due to pregnancy and childbirth, aging, chronic constipation, obesity, heavy lifting, or hormonal changes like menopause—problems can develop. Many people dismiss early signs as “normal” or feel embarrassed to mention them, delaying care until symptoms like incontinence or prolapse significantly interfere with daily life.
The good news? Identifying weak pelvic floor muscles early can prevent progression to more serious issues. By recognizing common warning signs and performing simple at-home self-checks, both men and women can take action before leaks, heaviness, or organ prolapse appear.
Spotting weakness early makes it much easier to address through targeted exercises, lifestyle changes, and professional guidance—helping you stay confident, active, and in control.Pelvic floor muscles form a hammock-like structure at the base of your pelvis, supporting the bladder, uterus (in women), prostate (in men), and rectum.
They play a crucial role in controlling urination, bowel movements, sexual function, and core stability. When these muscles weaken, problems like incontinence or prolapse can develop, but catching the issue early makes it much easier to address through simple exercises and lifestyle changes.
Why Early Identification Matters
Weak pelvic floor muscles often develop gradually due to factors such as pregnancy and childbirth, aging, chronic constipation, obesity, heavy lifting, or hormonal changes (like menopause). Many people dismiss early signs as “normal” or embarrassing, delaying care until symptoms interfere with daily life. Identifying weakness early prevents progression to more severe issues like pelvic organ prolapse or persistent incontinence.
The good news is that self-awareness and basic at-home checks can flag problems before they worsen, and strengthening is highly effective for most people.
Common Early Signs and Symptoms of Weak Pelvic Floor Muscles
Watch for these subtle indicators, especially if they appear after life events like childbirth, surgery, or weight gain:
- Light urinary leakage: Small leaks when coughing, sneezing, laughing, exercising, or lifting (known as stress incontinence). This is one of the most common early warnings.
- Urgency or frequency: Needing to urinate more than 8 times a day, waking multiple times at night (nocturia), or rushing to the bathroom with a sudden strong urge (urge incontinence).
- Incomplete emptying: Feeling like your bladder doesn’t fully empty after urinating, or needing to strain/push to start or finish.
- Bowel issues: Difficulty with constipation, straining to pass stool, accidental gas leakage, or fecal incontinence.
- Pelvic sensations: A feeling of heaviness, pressure, or dragging in the pelvis or vagina/rectum. In women, this might include a bulge sensation or tampons slipping out easily.
- Sexual changes: Reduced sensation during intercourse, difficulty achieving orgasm, or discomfort.
- Other clues: Lower back or tailbone pain, or a general sense that your core feels less stable during movement.
If several of these apply to you, especially if they’re new or worsening, it’s worth investigating further.
Simple At-Home Ways to Assess Pelvic Floor Strength
You can perform basic self-checks in private to gauge muscle function. These are not diagnostic but help you notice weakness early. Always consult a healthcare provider (such as a pelvic floor physical therapist, urogynecologist, or general doctor) for professional evaluation.
- Visual Check (Mirror Test): Sit with knees bent and use a handheld mirror to view the perineal area (between vagina and anus). Contract your pelvic floor as if stopping urine flow or holding gas. You should see a gentle inward and upward lift (the perineum draws up). No movement or outward bulging may indicate weakness.
- External Feel: Lie on your side with a pillow between your knees. Place fingers on the perineum. Contract the muscles—you should feel a tightening and slight lift under your fingers.
- Internal Self-Assessment (for Women): With clean hands and lubricant, insert one or two fingers into the vagina (up to the middle knuckle). Spread fingers slightly, then contract as if squeezing and lifting (like stopping urine or gripping a tampon). You should feel a squeeze around your fingers and an upward draw. Hold for 5–10 seconds if possible. Weakness shows as little to no squeeze, quick fatigue, or inability to lift.
- Endurance and Repetition Test: Contract the muscles, hold for 5 seconds, relax fully for 5 seconds, and repeat up to 10 times. Note how many quality repetitions you can do before the contraction weakens significantly. Also try a longer hold (aim for 10 seconds) to test endurance.
Important Notes on Self-Testing:
- Do not repeatedly stop urine flow mid-stream as a test or habit—this can lead to other issues.
- Focus on isolating the pelvic floor; avoid tightening your buttocks, thighs, or abdomen.
- Men can adapt these by contracting as if stopping urine or gas and feeling for lift at the base of the penis/scrotum.
- If you feel nothing or symptoms worsen, stop and seek professional help.
When to See a Professional
Don’t wait for symptoms to become severe. See a doctor or pelvic floor specialist if:
- You notice any leakage, bulging, or heaviness.
- Self-checks show poor contraction or coordination.
- Symptoms affect your quality of life, exercise, or confidence.
A specialist can perform a thorough exam, possibly including biofeedback or imaging, and rule out other conditions. Pelvic floor physical therapy is often the first-line treatment and highly successful when started early.
Next Steps: Strengthening and Prevention
If weakness is suspected, start with gentle Kegel exercises (after confirming proper technique):
- Squeeze and lift the pelvic floor for 3–5 seconds, relax for the same time.
- Build to 10–15 repetitions, 3 times daily, in different positions (lying, sitting, standing).
- Combine with proper breathing—exhale on the squeeze, avoid breath-holding.
- Progress gradually and consider working with a therapist for personalized guidance, as some people need relaxation techniques first if muscles are tight rather than purely weak.
Lifestyle tips for prevention and support:
- Maintain a healthy weight and avoid chronic straining (treat constipation with fiber and hydration).
- Lift properly using your legs and core.
- Stay active with low-impact exercises like walking, swimming, or Pilates.
- During/after pregnancy, prioritize pelvic floor care.
Early action on pelvic floor health can restore control, boost confidence, and prevent bigger problems. Listen to your body, perform occasional self-checks, and don’t hesitate to seek expert support—most issues improve dramatically with the right approach. If you’re experiencing symptoms, talk to a healthcare provider soon for tailored advice.
Here’s a clear, evidence-based discussion of the most common myths surrounding pelvic floor muscles and health. Many people delay care or try ineffective fixes because of these misconceptions. Understanding the facts can help you take better care of your body—whether you’re male, female, young, old, or anywhere in between.
Myth 1: Pelvic Floor Issues Are Only a Women’s Problem (Especially After Childbirth)
Fact: Everyone has a pelvic floor. Men, women, and even children can experience pelvic floor dysfunction. While pregnancy and vaginal birth are major risk factors for women, men can develop issues like post-prostate surgery incontinence, chronic pelvic pain, or erectile difficulties due to pelvic floor problems. Athletes, people with chronic constipation, obesity, heavy lifting jobs, or chronic cough can also be affected regardless of gender or reproductive history.
Childbirth increases risk, but it’s not the only cause—and not everyone who gives birth will have problems.
Myth 2: Pelvic Floor Dysfunction Is Normal (or Inevitable) with Aging, Pregnancy, or Childbirth
Fact: Symptoms like leaking urine when coughing/sneezing, a feeling of heaviness in the pelvis, or pain during sex are common but not normal. They are signs that something needs attention. Many issues can be prevented, significantly improved, or fully resolved with proper care, even years later. Accepting leakage as “just part of being a mom” or “getting older” often leads to unnecessary suffering.
Pregnancy itself puts pressure on the pelvic floor, but dysfunction isn’t inevitable. C-sections do not fully protect against pelvic floor problems because the weight of the baby during pregnancy is already a factor.
Myth 3: Kegel Exercises Are the Universal Fix—Just Do More of Them
Fact: Kegels (pelvic floor contractions) can help when muscles are truly weak and need strengthening, but they are not appropriate for everyone. Many people actually have overactive or tight pelvic floor muscles rather than weak ones. Doing Kegels in this case can worsen pain, urgency, or constipation.
Up to 50% of people perform Kegels incorrectly when given only verbal instructions, which can lead to no improvement or even more problems. Proper technique, coordination with breathing, and sometimes focusing on relaxation first are crucial. Pelvic floor physical therapy often includes manual therapy, breathing work, posture correction, and functional exercises—not just endless squeezes.
Bonus related myth: Stopping the flow of urine mid-stream is a good way to practice or test Kegels. Experts generally advise against making this a habit, as it can disrupt normal bladder function.
Myth 4: Pelvic Floor Physical Therapy Is Only for Postpartum Women or Severe Cases
Fact: Pelvic floor PT benefits people of all genders and life stages—athletes with hip/back pain, men with post-prostate issues, teens with constipation, people in menopause, or anyone with pelvic pain. You don’t need to wait until symptoms are debilitating. Early intervention often leads to faster, better results and can prevent worsening.
Therapy goes far beyond Kegels. It may involve biofeedback, stretching tight muscles, strengthening the core and glutes in coordination, or addressing scar tissue and posture.
Myth 5: If You Have No Obvious Symptoms, Your Pelvic Floor Is Fine
Fact: The pelvic floor contributes to core stability, sexual function, bowel/bladder health, and even lower back/hip function. Subtle issues can show up as lower back pain, poor posture during exercise, reduced orgasm intensity, or a general feeling of core instability long before major leakage or prolapse occurs. Regular awareness (like the self-checks discussed previously) helps catch problems early.
Myth 6: Once You Finish Pelvic Floor Therapy (or Have a Baby), You Don’t Need to Maintain It
Fact: Pelvic floor health requires ongoing attention, just like any other muscle group. Lifestyle factors—maintaining healthy weight, avoiding chronic straining, lifting with good technique, staying active, and managing constipation—play a big role in long-term success. Many people benefit from occasional “tune-ups” or continuing simple, individualized exercises.
Why These Myths Persist and What to Do Instead
These myths often stem from embarrassment, outdated advice, or the assumption that “common = normal.” The reality is that effective, non-surgical help is available for most pelvic floor concerns. A specialized pelvic floor physical therapist is usually the best first step—they can assess whether your muscles are weak, tight, uncoordinated, or a mix, and create a personalized plan.
Key takeaways:
- Listen to your body: Any new leakage, pressure, pain, or changes in bowel/bladder/sexual function deserves attention.
- Don’t self-diagnose and endlessly Kegel—get a proper assessment.
- Men and non-postpartum people: You’re not alone, and help exists.
- Early action usually means simpler, faster improvement.
If you’re experiencing symptoms (even mild ones), talk to your doctor or seek a pelvic health specialist. Most people see significant improvement with the right guidance, and you don’t have to accept discomfort as your new normal.
Pelvic floor health is an important part of overall wellness at every age and stage. Busting these myths is the first step toward feeling stronger, more confident, and in better control.
Disclaimer This article is for informational and educational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. The self-assessment techniques and information provided here are general in nature and may not be suitable for everyone.
Pelvic floor health concerns can vary widely between individuals. Always consult a qualified healthcare provider, such as your doctor, urogynecologist, or a specialized pelvic floor physical therapist, before attempting any self-checks, exercises, or lifestyle changes—especially if you are pregnant, postpartum, recovering from surgery, or experiencing pain, bleeding, or other concerning symptoms.
If you notice any signs of weak pelvic floor muscles (such as leakage, heaviness, or discomfort), seek personalized medical evaluation promptly. Do not rely solely on this or any online content for your health decisions. Results from self-assessments or exercises can differ, and improper technique may lead to further issues.
The author and publisher are not liable for any injuries, damages, or health outcomes that may arise from the use of this information.