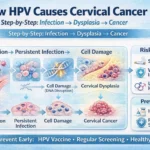
Nearly 100% of cervical cancers are caused by persistent infection with high-risk types of human papillomavirus (HPV) . Because we know the cause, we have developed an arsenal of prevention strategies—from the powerful HPV vaccine to lifestyle changes that boost your body’s natural defenses. This article brings together the best of both worlds: medical interventions that provide a shield against the virus, and natural approaches that strengthen your immune system to fight infection and maintain cervical health.
Whether you are a young woman considering the HPV vaccine, a mother making decisions for your children, or someone looking to adopt healthier habits, this guide is for you. Let us begin.
Chapter 1: Understanding Cervical Cancer – The HPV Connection
Before diving into prevention, it is essential to understand what we are preventing. Cervical cancer develops in the cells of the cervix—the lower part of the uterus that opens into the vagina. The disease does not appear overnight. It progresses slowly over 10 to 20 years, starting with precancerous changes called dysplasia or cervical intraepithelial neoplasia (CIN) .
The Role of HPV
Human papillomavirus (HPV) is the most common sexually transmitted infection in the United States. Most sexually active people will contract HPV at some point in their lives . There are more than 200 types of HPV, but only about 14 are considered “high-risk” for causing cancer. HPV types 16 and 18 alone are responsible for approximately 70% of all cervical cancers .
Here is the crucial nuance: Most HPV infections clear on their own. The human immune system is remarkably effective at eliminating the virus within 1 to 2 years . The problem arises when the infection persists. Persistent infection with high-risk HPV types can cause changes in cervical cell DNA, leading to precancerous changes that may eventually develop into cancer if left untreated .
Because we understand this pathway, we have multiple opportunities to intervene:
| Stage of HPV-Cervical Cancer Pathway | Prevention Strategy |
|---|---|
| Before HPV exposure | HPV vaccine |
| After HPV infection but before persistent infection | Strong immune system (diet, exercise, stress reduction, no smoking) |
| Precancerous changes (dysplasia) | Regular screening (Pap test, HPV test) |
| Early-stage cancer | Treatment (still highly curable) |
The goal of prevention is to stop the process as early as possible—ideally before HPV infection even occurs.
Chapter 2: The Role of HPV Vaccine in Prevention – Your Shield Against Cancer
The HPV vaccine is, without exaggeration, one of the most significant advances in cancer prevention in human history. It is a cancer prevention vaccine—a concept that was almost unimaginable a generation ago.
What Does the HPV Vaccine Do?
The HPV vaccine protects against the types of HPV that most often cause cervical, vaginal, and vulvar cancers. The currently available vaccine in the United States is Gardasil 9, which protects against nine HPV types, including the two highest-risk types (16 and 18) responsible for about 90% of cervical cancers .
The vaccine works by causing your body to produce antibodies against the virus. It prevents new HPV infections but does not treat existing infections or diseases . This is why the vaccine works best when given before any exposure to HPV—ideally before sexual activity begins.
Who Should Get the HPV Vaccine?
| Age Group | Recommendation | Doses |
|---|---|---|
| Ages 9–14 | Recommended for all children | 2 doses, 6–12 months apart |
| Ages 15–26 | Catch-up vaccination recommended | 3 doses (0, 2, and 6 months) |
| Ages 27–45 | May benefit; discuss with doctor | 3 doses if indicated |
According to the CDC, HPV vaccination is recommended for preteens aged 11 to 12 years, but can be given starting at age 9 . The American Cancer Society (ACS) recommends vaccination for everyone through age 26 who is not already vaccinated .
For adults aged 27 through 45 who are not already vaccinated, the CDC notes that vaccination provides less benefit because most people in this age range have already been exposed to HPV. However, some adults in this age group may decide to get the HPV vaccine after speaking with their doctor about their risk for new HPV infections and the possible benefits of vaccination .
How Effective Is the HPV Vaccine?
The data on HPV vaccine effectiveness is remarkable:
- The vaccine is nearly 100% effective at preventing precancerous cervical changes and cervical cancers caused by the HPV types it targets when given before exposure to the virus
- Studies have shown HPV infections have decreased by 88% among teen girls and 81% among young adult women since the vaccine was introduced
- Countries with high vaccination rates have seen cervical cancer rates decline by up to 87%
- Protection appears to last at least 12+ years, and studies suggest it may be lifelong
Is the HPV Vaccine Safe?
Yes. The HPV vaccine has undergone extensive safety testing and has been administered more than 270 million doses worldwide . The most common side effects are mild and temporary, including pain, redness, or swelling at the injection site, headache, and low-grade fever . Serious side effects are extremely rare.
The vaccine is typically given as a shot in the muscle of the upper arm or upper leg . Your doctor may ask you to stay for about 15 minutes after the injection to monitor for any immediate reactions.
Important Note: Vaccination Does Not Replace Screening
Even if you have received the HPV vaccine, you must continue regular cervical cancer screening. The vaccine does not protect against all HPV types that can cause cervical cancer, and it does not treat existing infections . Screening remains an essential part of prevention.
Chapter 3: Cervical Cancer Screening – Your Safety Net
Screening is the second pillar of cervical cancer prevention. While the vaccine prevents infection, screening detects precancerous changes early—when treatment is nearly 100% effective.
Types of Screening Tests
There are two main screening tests:
| Test | What It Detects | How Often (for average risk) |
|---|---|---|
| Pap test (Pap smear) | Precancerous cell changes (dysplasia) | Every 3 years (ages 21–65) |
| HPV test | Presence of high-risk HPV types | Every 5 years (ages 30–65) |
| Co-testing | Both Pap and HPV tests together | Every 5 years (ages 30–65) |
The Pap test looks for precancers—cell changes on the cervix that might become cervical cancer if not treated appropriately. The HPV test looks for the virus that can cause these cell changes .
Screening Guidelines (U.S.)
According to the American College of Obstetricians and Gynecologists and the U.S. Preventive Services Task Force:
- Ages 21–29: Pap test every 3 years. HPV testing is not recommended for this age group because HPV infections are common and usually clear on their own .
- Ages 30–65: Options include an HPV test every 5 years, a Pap test every 3 years, or co-testing (both tests) every 5 years .
- Over age 65: Screening may stop if you have had 3 normal Pap tests in a row (or 2 normal HPV tests) within the past 10 years and are not otherwise at high risk for cervical cancer .
- Women who have had a hysterectomy with removal of the cervix and no history of cervical cancer or precancer generally do not need screening .
What If You Have Abnormal Results?
An abnormal screening result does not mean you have cancer. It means further evaluation is needed. The next step is often a colposcopy—a closer examination of the cervix using a special magnifying instrument. If precancerous changes are found, they can be removed in a simple office procedure, preventing cancer from ever developing.
CDC Free or Low-Cost Screening
If cost is a concern, the CDC offers free or low-cost cervical cancer screening tests through the National Breast and Cervical Cancer Early Detection Program . Do not let financial barriers prevent you from getting screened.
Chapter 4: Lifestyle Changes That Protect Cervical Health (Naturally)
While the HPV vaccine and regular screening are the cornerstones of prevention, your daily choices play a powerful supporting role. A healthy lifestyle strengthens your immune system, helping your body clear HPV infections naturally and maintain healthy cervical cells.
4.1 Quit Smoking – The Single Most Important Lifestyle Change
If you smoke, quitting is the most powerful lifestyle change you can make to reduce your cervical cancer risk.
Why it matters: Women who smoke are about twice as likely to develop cervical cancer as non-smokers . Tobacco carcinogens concentrate in cervical mucus, directly damaging cervical cell DNA and weakening the body’s ability to fight off HPV infections .
The good news: Quitting smoking gradually reduces your risk over time. Research suggests that your risk approaches that of never-smokers after about 10 to 15 years of being smoke-free .
Actionable steps: Talk to your doctor about smoking cessation programs, nicotine replacement therapy, or prescription medications that can help you quit.
4.2 Eat a Cervix-Protecting Diet
What you eat directly affects how well your immune system functions and how your cells repair themselves. A nutrient-rich diet provides the building blocks your body needs to fight HPV and repair damaged cells.
Power Nutrients for Cervical Health
| Nutrient | Why It Helps | Food Sources |
|---|---|---|
| Folate (Vitamin B9) | Repairs DNA and prevents cell mutations | Leafy greens (spinach, kale), lentils, avocado, asparagus |
| Vitamin C | Boosts immunity and supports tissue repair | Citrus fruits, berries, bell peppers, kiwi, broccoli |
| Vitamin E | Protects cells from oxidative damage | Nuts, seeds, spinach, sunflower oil |
| Beta-carotene (Vitamin A) | Keeps cervical tissue healthy | Carrots, sweet potatoes, kale, butternut squash |
| Selenium | Supports immune function and hormone balance | Brazil nuts (just 2–3 per day!), seafood, eggs |
| Zinc | Strengthens immune response | Pumpkin seeds, chickpeas, cashews, shellfish |
Superfoods for Cervical Health
Certain foods deserve special mention for their protective properties:
- Cruciferous vegetables (broccoli, cauliflower, cabbage, kale): Contain sulforaphane, a compound that helps detoxify harmful substances and fight abnormal cells .
- Green tea: Rich in catechins (antioxidants) that may help inhibit HPV activity .
- Turmeric: Contains curcumin, a powerful anti-inflammatory and antiviral compound .
- Garlic and onions: Nature’s antimicrobials that give your immune system a boost .
- Fatty fish (salmon, sardines): Deliver omega-3 fatty acids that calm inflammation throughout your body .
Foods to Limit or Avoid
Just as some foods protect your cervix, others work against you:
- Processed meats (hot dogs, sausages): Contain nitrates and preservatives linked to cancer risk
- Refined sugars and white flour: Feed harmful gut bacteria and weaken immunity
- Fried and fast foods: Promote inflammation throughout your body
- Excessive alcohol: Impairs liver function and immunity
Practical tip: Do not try to change everything overnight. Start by adding one or two protective foods to your meals each day, and gradually reduce the less healthy options.
4.3 Support Your Gut Health
Your gut health and cervical health are more connected than you might think. A healthy gut microbiome strengthens your immune system and supports your body’s ability to clear HPV .
To support your gut:
- Eat fermented foods like yogurt, kimchi, sauerkraut, and kefir
- Include fiber-rich foods such as fruits, vegetables, legumes, and whole grains
- Limit processed foods and sugar
- Stay well hydrated
4.4 Exercise Regularly
Physical activity is medicine for your entire body, including your cervix. According to research published in the Journal of Lower Genital Tract Disease, individuals who did not get regular physical activity had an increased risk of cervical cancer .
Recommendation: Aim for at least 150 minutes of moderate exercise weekly—that is about 30 minutes per day, five days a week. Brisk walking, swimming, cycling, and yoga all count .
Exercise boosts circulation, strengthens immunity, helps maintain a healthy weight, and keeps your hormones balanced.
4.5 Manage Stress
Chronic stress quietly weakens your immune system, making it harder for your body to fight off HPV. Finding ways to calm your mind is not just good for your mental health—it is essential for your cervical health as well .
Stress-reduction techniques that work:
- Deep breathing exercises
- Meditation or mindfulness
- Journaling
- Adequate sleep (7–9 hours per night)
- Spending time in nature
- Connecting with loved ones
Even 10 minutes of daily stress relief can help your immune system work more effectively .
4.6 Practice Safe Sex
Since HPV is transmitted through skin-to-skin contact during sexual activity, safe sex practices can reduce your risk of exposure.
Strategies that help:
- Use condoms consistently and correctly during every sexual act. While condoms do not cover all possible HPV-infected areas, they reduce the risk of transmission .
- Limit the number of sexual partners you have over your lifetime .
- Mutual monogamy with a partner who has been tested reduces risk.
- Delay first intercourse if possible (early sexual activity increases HPV exposure risk) .
4.7 Maintain a Healthy Weight
Obesity can alter hormone levels and impair immune function, modestly increasing cervical cancer risk . Maintaining a healthy weight through diet and exercise is an important part of an overall prevention strategy.
Chapter 5: Putting It All Together – Your Cervical Health Action Plan
Prevention is most effective when you combine medical interventions with healthy lifestyle habits. Here is your step-by-step action plan.
For Young Women and Parents of Preteens (Ages 9–26)
| Action | Timeline |
|---|---|
| Get the HPV vaccine | Start at age 9–12; complete the series |
| Establish healthy habits | Diet, exercise, no smoking—start now |
| Learn about screening | Know that screening starts at age 21 |
For Women Ages 21–29
| Action | Timeline |
|---|---|
| Pap test | Every 3 years |
| Continue healthy lifestyle | Daily |
| HPV vaccine if not already vaccinated | Catch-up doses available |
For Women Ages 30–65
| Action | Timeline |
|---|---|
| HPV test | Every 5 years, OR |
| Pap test | Every 3 years, OR |
| Co-testing (both) | Every 5 years |
| Follow up on any abnormal results | Immediately |
| Continue healthy lifestyle | Daily |
For All Women
| Action | Why |
|---|---|
| Do not smoke | Single most important lifestyle change |
| Eat a nutrient-rich diet | Supports immune function and cell repair |
| Exercise 150 minutes/week | Boosts immunity and reduces inflammation |
| Manage stress | Chronic stress weakens immune response |
| Practice safe sex | Reduces HPV exposure risk |
| Get enough sleep (7–9 hours) | Sleep is when your body repairs itself |
Chapter 6: Frequently Asked Questions
Can a healthy diet alone prevent cervical cancer?
While a nutrient-rich diet strengthens your immune system and helps your body fight HPV, it cannot guarantee cervical cancer prevention on its own. The most effective approach combines healthy eating with regular Pap smears, HPV vaccination (if eligible), and lifestyle habits like not smoking. Think of diet as one powerful tool in your overall prevention strategy, not a replacement for medical screening .
Can you get cervical cancer if you have had the HPV vaccine?
While the HPV vaccine significantly reduces cervical cancer risk, it does not protect against all HPV types that can cause cancer. This is why regular screening is still recommended even for vaccinated women. However, the vaccine targets the HPV types responsible for about 90% of cervical cancers .
How often should I get screened for cervical cancer?
Most women should have a Pap test every 3 years starting at age 21. From age 30, you have options: a Pap test every 3 years, an HPV test every 5 years, or co-testing (both) every 5 years. Your doctor may recommend more frequent screening based on your individual risk factors .
Does using condoms prevent HPV?
Condoms provide some protection against HPV but do not eliminate the risk entirely. This is because HPV can infect areas not covered by a condom. However, consistent condom use has been associated with a lower rate of cervical cancer .
Can herbal remedies or supplements help prevent cervical cancer?
Certain herbs and nutrients show promise for cervical health—green tea extracts, turmeric (curcumin), and mushroom extracts have demonstrated immune-boosting and antiviral properties in some studies. However, they work best as additions to—not replacements for—medical screening and a healthy diet. Always consult your doctor before starting any new supplement .
What are the warning signs of cervical cancer?
Early-stage cervical cancer often causes no symptoms. This is why screening is so important. When symptoms do appear, they may include:
- Abnormal vaginal bleeding (after intercourse, between periods, or after menopause)
- Unusual vaginal discharge (watery, bloody, or with a foul odor)
- Pelvic pain not related to menstruation
- Pain during sexual intercourse
If you experience any of these symptoms, see your healthcare provider promptly .
Conclusion: You Have the Power to Prevent
Cervical cancer is one of the few cancers that we have the tools to nearly eliminate. The HPV vaccine can prevent the infections that cause the vast majority of cases. Regular screening can catch precancerous changes years before they become cancer. And healthy lifestyle choices—quitting smoking, eating well, exercising, managing stress—strengthen your body’s natural defenses.
The tragedy is not that we lack these tools. The tragedy is that too many women are still not using them. According to the CDC, most people who are diagnosed with cervical cancer have not been screened recently .
Do not let that be you. Do not let that be someone you love.
Take action today:
- If you or your children are within the recommended age range, get the HPV vaccine.
- Schedule your screening if you are due.
- Quit smoking—your cervix will thank you.
- Add one protective food to your diet this week.
- Share this information with the women in your life.
Cervical cancer is preventable. You have the power to protect yourself. Use it.
Summary Table: Prevention Strategies at a Glance
| Strategy | What to Do | How Often |
|---|---|---|
| HPV Vaccine | Complete the vaccine series | Once (ages 9–26; discuss with doctor up to age 45) |
| Pap Test | Cervical cell screening | Every 3 years (ages 21–65) |
| HPV Test | Virus detection | Every 5 years (ages 30–65) |
| Quit Smoking | Stop tobacco use | One time (lifelong benefit) |
| Healthy Diet | Eat fruits, vegetables, whole grains | Daily |
| Exercise | 30 minutes moderate activity | 5 days per week |
| Stress Management | Meditation, sleep, social connection | Daily |
| Safe Sex | Condoms, limit partners | Every sexual encounter |
Call to Action
Your health is in your hands. If you are due for a Pap test or HPV test, call your doctor today. If you or your child has not received the HPV vaccine, schedule an appointment. Small actions now can prevent cancer years from now. Do not wait. Your future self will thank you.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider for medical advice, diagnoses, or treatment. The HPV vaccine and screening recommendations may vary based on individual health history and risk factors.