You have heard the statistic before. A consanguineous marriage—defined as a union between second cousins or closer—raises the risk of birth defects from approximately 2-3% to 4-6%. For generations, that was the only number that mattered. Families in North Africa, the Middle East, South Asia, and beyond weighed that modest increase against centuries of tradition, economic stability, and cultural cohesion.
But what if that 4-6% figure is dangerously incomplete? What if the true genetic risk of marriage consanguinity lies not in the handful of recessive mutations that carrier panels detect, but in the thousands of common variants that those panels cannot see?
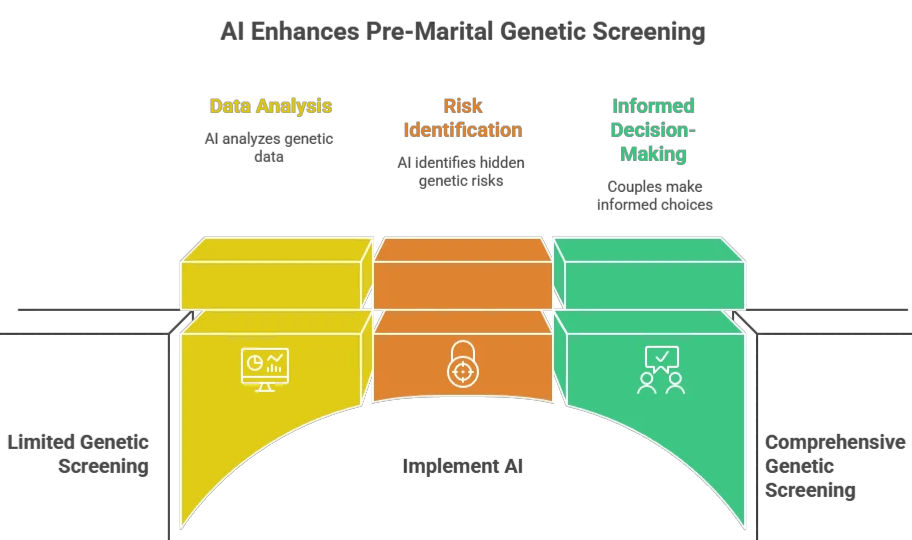
Welcome to Pre-Marital Genetic Screening 2.0—where artificial intelligence, polygenic risk scores, and population genomics converge to give consanguineous marriages something they have never had before: a complete, predictive, and actionable roadmap. Stop guessing. Start preventing.
Chapter 1: What Is Consanguineous Marriage? Beyond the Dictionary
Before we discuss the AI revolution, we must first answer a fundamental question: what is consanguineous marriage? The consanguineous marriage definition is deceptively simple. Biologically, it refers to a union between individuals who share a common ancestor within the last four to five generations. Practically, this means second cousins or closer.
The consanguineous marriage meaning , however, extends far beyond biology. In many cultures, to define consanguineous marriage is to describe a social contract that preserves wealth, strengthens tribal alliances, simplifies matchmaking, and ensures shared religious and moral values.
If you ask a geneticist to define consanguineous marriage, they will calculate the inbreeding coefficient (F)—the probability that an offspring inherits two identical copies of a gene from a common ancestor. For first cousins, F = 0.0625 (6.25%). For second cousins, F = 0.0156 (1.56%). These numbers are small but meaningful.
But here is the critical insight that traditional definitions miss. When we define consanguineous marriage solely by its recessive mutation risk, we ignore the elephant in the room: genome-wide homozygosity. Offspring of consanguineous marriages inherit longer stretches of DNA where both chromosomes are identical.
Those stretches can harbor not just rare, catastrophic mutations, but also thousands of common, small-effect variants that cumulatively raise the risk of diabetes, heart disease, schizophrenia, and autoimmune disorders. That is why the old consanguineous marriage meaning needs an urgent update.
What is consanguineous marriage in the era of genomic medicine? It is no longer just a cultural practice with a small statistical risk. It is a unique genetic architecture that AI can now decode, predict, and mitigate.
Chapter 2: The Failure of Traditional Screening
Today, a typical pre-marital genetic screen for a consanguine marriage looks like this: a blood draw, a panel of 50 to 500 known recessive disease genes, and a binary result—”carrier” or “non-carrier.” If both partners carry a mutation in the same gene, they are offered prenatal diagnosis or PGD. If not, they are given a green light.
This approach, while valuable, is essentially 1.0 technology. It suffers from four fatal flaws:
Flaw 1: It Only Sees Rare Diseases
Traditional panels screen for conditions like cystic fibrosis, spinal muscular atrophy, and beta-thalassemia—diseases that affect fewer than 1 in 10,000 people. They are completely blind to common complex diseases that affect millions.
Flaw 2: It Ignores Homozygosity Burden
Two first cousins may carry zero shared recessive mutations. But they still share 12.5% of their genome identical by descent. That shared DNA contains thousands of SNPs. Some of those SNPs are harmless. Others, when homozygous, increase disease risk. Traditional screening sees none of them.
Flaw 3: It Has No Predictive Power for Polygenic Conditions
A couple with a family history of diabetes or heart disease gets no actionable information from a recessive panel. They are told, “Your child won’t have Tay-Sachs.” But they are not told, “Your child has a 40% higher lifetime risk of type 2 diabetes due to homozygosity at 15 risk loci.”
Flaw 4: It Is Culturally Static
Traditional screening offers a single solution: avoidance or termination. It does not offer prevention, monitoring, or lifestyle modification. For families deeply committed to consanguinity marriage as a social and religious value, this binary choice is often rejected outright.
Enter AI. Enter Pre-Marital Screening 2.0.
Chapter 3: The AI Revolution – How Machine Learning Predicts Risk
Artificial intelligence is not a magic wand. It is a pattern-matching engine. When trained on massive genomic datasets from consanguineous marriages, AI can learn to predict outcomes that no single gene test can reveal. Here is how it works.
Step 1: Build a Consanguinity-Aware Genome Database
Most genomic reference data comes from outbred European populations. Those data are useless for marriage consanguinity because the patterns of linkage disequilibrium, allele frequencies, and homozygosity runs are completely different. The first step of Pre-Marital Screening 2.0 is to sequence hundreds of thousands of individuals from populations where consanguineous marriages are common—Saudi Arabia, Pakistan, Turkey, Egypt, and parts of India. This creates a reference panel that reflects reality.
Step 2: Train Deep Learning Models on Runs of Homozygosity (ROH)
AI models are fed millions of data points: the length, location, and gene content of each ROH in an individual’s genome. The model learns that a long ROH on chromosome 6p22 is associated with a 15% increased risk of schizophrenia. Another ROH on chromosome 9p21 raises cardiovascular risk by 22%. These associations are invisible to traditional screening because they involve common variants, not rare mutations.
Step 3: Generate a Unified Risk Score
For a given consanguineous couple, the AI model integrates:
- Traditional recessive mutation carrier status
- Polygenic risk scores for 20+ common diseases
- ROH burden across the entire genome
- Family history data (structured and unstructured, extracted from clinical notes using NLP)
- Ethnicity-specific allele frequencies
The output is not a single number. It is a dynamic, interactive report that shows predicted risk percentiles for each disease, with confidence intervals and actionable recommendations.
Step 4: Simulate Offspring Genomes
This is the true revolution. Using the couple’s phased genomes, AI can simulate 10,000 or 100,000 virtual offspring. For each simulation, it calculates the expected ROH burden, polygenic risk scores, and recessive mutation status. The couple can see, with statistical power, the range of possible outcomes for their future children. No more guessing. No more “4-6%” generalizations. Just personalized, predictive data.
Chapter 4: Real-World Case Study – Ahmed and Fatima
Let us make this concrete. Ahmed and Fatima are first cousins from a Moroccan Berber community. They are deeply in love and committed to their consanguineous marriage . Their families have practiced marriage consanguinity for five generations. They come for pre-marital screening expecting the standard panel.
Traditional Screening Result:
- Recessive panel: Clear. No shared mutations.
- Counselor’s advice: “Your risk is only slightly elevated. Proceed.”
Pre-Marital Screening 2.0 Result (AI-Powered):
- Recessive panel: Still clear.
- Polygenic risk scores (consanguinity-adjusted):
- Type 2 diabetes: 82nd percentile (1.7x population risk)
- Coronary artery disease: 74th percentile (1.4x risk)
- Schizophrenia: 68th percentile (1.3x risk)
- ROH burden: 225 Mb of homozygous sequence (higher than 90% of outbred couples)
- Simulation of 10,000 virtual offspring:
- 12% will have a PRS for diabetes above the 90th percentile
- 8% will have a PRS for CAD above the 90th percentile
- 0.3% will have a recessive disorder (already known)
Actionable Recommendations (AI-Generated):
- Lifestyle: Enroll all children in a low-glycemic, Mediterranean-style diet from age 5.
- Monitoring: Yearly HbA1c starting at age 25. Coronary calcium score at age 40.
- Pharmacologic: Consider metformin prophylaxis for any child with BMI > 25 and family history.
- Psychiatric: Baseline cognitive assessment at age 18. Low-threshold intervention for any mood symptoms.
Ahmed and Fatima do not cancel their wedding. They proceed with eyes wide open, armed with a 20-year prevention plan. That is Pre-Marital Screening 2.0.
Chapter 5: The Meaning of Consanguinity – Cultural Competence Meets AI
To define consanguineous marriage as purely a medical risk is to misunderstand its soul. In many communities, when you ask what is consanguineous marriage, the answer is not about genes. It is about trust. It is about a father knowing his daughter will be treated well because she is marrying her cousin. It is about property staying within the family. It is about shared holidays, shared grief, and shared joy.
Any AI system that ignores this cultural reality will fail. Not because the science is wrong, but because no one will use it.
Pre-Marital Screening 2.0 must be co-designed with community elders, religious scholars, and traditional matchmakers. The interface must be available in Arabic, Urdu, Turkish, and French. The risk communication must use visual analogies, not intimidating percentiles. And the recommendations must never suggest that consanguineous marriages are inferior. They must simply say: “Here is your map. Here are the roads with higher traffic. Here is how to drive safely.”
The consanguineous marriage meaning in 2025 is not “risky.” It is “navigable.”
Chapter 6: The Ethical Guardrails – What AI Must Never Do
With great predictive power comes great ethical responsibility. Pre-Marital Screening 2.0 must operate within strict guardrails.
Guardrail 1: No Embryo Selection for Polygenic Traits
The system must never output a “ranked list” of simulated embryos for non-medical traits. That is the road to eugenics. PRS for height, IQ, or eye color must be excluded entirely.
Guardrail 2: No Denial of Marriage Licenses
A high polygenic risk score is not a reason to prohibit a consanguine marriage. It is a reason to offer enhanced preventive care. The goal is empowerment, not prohibition.
Guardrail 3: Informed Consent Must Be Real
Couples must understand that PRS predictions are probabilistic, not deterministic. A high PRS for breast cancer does not mean cancer will occur. A low PRS does not guarantee health. The AI must display confidence intervals and explain that environmental factors often outweigh genetics.
Guardrail 4: Data Sovereignty
Genomic data from communities that practice marriage consanguinity must not be exploited by Western biotech companies without benefit-sharing agreements. Local researchers must lead. Local communities must consent.
Chapter 7: The Road Ahead – From 2.0 to 3.0
Pre-Marital Screening 2.0 is not science fiction. The first prototypes are already running in research settings in Qatar, Saudi Arabia, and Pakistan. Within five years, commercial versions will be available.
But even 2.0 is a stepping stone. Version 3.0 will integrate:
- Epigenetic clocks to predict biological aging trajectories
- Gut microbiome sequencing from stool samples to predict metabolic disease
- Polyenvironmental risk scores combining genetic data with air quality, water quality, and socioeconomic data
- Federated learning models that train across borders without sharing raw genomic data
For a consanguineous couple in 2030, pre-marital screening will not be a single blood test. It will be a comprehensive health forecast for their entire future family line.
Conclusion: Redefining the Meaning of Consanguinity
Let us return to where we began. What is consanguineous marriage? For centuries, the answer was cultural. Then, for a few decades, the answer became medical and fearful. Now, with AI-powered pre-marital screening, we have the chance to offer a third answer.
Consanguineous marriage meaning is not destiny. It is not a curse. It is a genetic architecture—one that AI can understand, predict, and mitigate. The consanguineous marriage definition for the 21st century should read: A union between relatives that, when combined with genomic intelligence, becomes an opportunity for precision prevention rather than a gamble.
To define consanguineous marriage in the age of AI is to say this: Yes, there is risk. But there is also a map. There is a plan. There is hope.
Consanguine marriage will not disappear. It will evolve. And with Pre-Marital Screening 2.0, it will become safer, smarter, and more respectful of the families who have trusted it for generations.
Stop guessing. Start screening. Start preventing.
*If you are planning a consanguineous marriage, do not settle for a 20th-century blood test. Ask your genetic counselor: “Can you calculate our polygenic risk scores? Can you simulate our offspring? Can you give us a prevention plan, not just a probability?” If the answer is no, find a clinic that offers Pre-Marital Screening 2.0. Your children’s future health depends on it.*