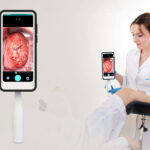
Introduction: A Turning Point in Women’s Health
Cervical cancer prevention relies on early detection and advanced screening technologies. Regular Pap smears and HPV testing help identify abnormal cells before they become cancerous. New innovations such as AI-powered diagnostics, self-sampling HPV kits, and molecular biomarkers are making screening more accurate and accessible. By combining routine screening with modern tools, cervical cancer can be detected early—or prevented entirely.
How to Prevent Cervical Cancer Early:
- Get regular Pap smear screenings
- Take HPV tests for high-risk virus detection
- Consider HPV vaccination for long-term protection
- Use self-sampling kits if clinic access is limited
- Leverage AI-based and advanced diagnostic tools for accurate results
- Follow up early on abnormal findings
What is the best way to detect cervical cancer early?
The most effective way to detect cervical cancer early is through routine Pap smears and HPV testing, which identify abnormal cervical cells before they turn cancerous. Emerging technologies like AI-assisted screening and biomarker testing further improve accuracy and early diagnosis.
Cervical cancer can be prevented through early detection using Pap smears, HPV testing, and advanced screening technologies like AI diagnostics and self-sampling kits, allowing treatment before cancer develops.
Cervical cancer remains one of the most preventable yet dangerously overlooked diseases affecting women worldwide. The real threat isn’t just the disease itself—it’s the deadly silence in which it develops. Most women experience no early symptoms, allowing abnormal cervical changes to progress unnoticed until they become far more difficult to treat. This gap between hidden danger and late diagnosis is where lives are often lost.
But the landscape is rapidly changing.

We are now entering an era where missed diagnosis is being replaced by early, precise detection. From proven screening tools like Pap smears and HPV testing to cutting-edge innovations such as AI-powered diagnostics, portable screening devices, and molecular biomarkers, cervical health is undergoing a powerful transformation. These advancements are shifting the focus from reactive treatment to proactive prevention and early defense.
Today, the question is no longer “Can cervical cancer be detected early?”—but rather, “Are we using the right tools at the right time?”
This guide explores powerful cervical health strategies, combining established screening methods with next-generation technologies, to help both individuals and healthcare providers identify risks earlier, act faster, and prevent progression effectively. Whether you’re looking to understand warning signs, improve screening outcomes, or stay ahead with future-ready diagnostics, the solutions are now more accessible—and more impactful—than ever before.
Cervical cancer is one of the few malignancies that modern medicine can prevent entirely. Yet paradoxically, it remains the fourth most common cancer in women globally, with an estimated 660,000 new cases in 2022—94% of which occurred in low- and middle-income countries . This disparity reveals a fundamental truth: while the science of cervical disease prevention is well-established, access to that science remains profoundly unequal.
The story of cervical health is one of transformation. Over the past five decades, we have moved from treating invasive cancer to detecting precancerous changes before they become malignant. Today, we stand at the threshold of an even more dramatic shift—from cytology-based screening (looking at cells under a microscope) to molecular and AI-driven diagnostics that promise greater accuracy, accessibility, and patient empowerment.
This comprehensive guide explores the full spectrum of cervical health: from basic anatomy and the natural history of HPV infection to the limitations of traditional screening and the emerging technologies—biomarkers, artificial intelligence, microbiome science, and at-home testing—that are reshaping how we prevent cervical cancer.
Part 1: Understanding the Cervix – Anatomy and Function
What Is the Cervix?
The cervix is the lower, narrow end of the uterus that connects the uterine cavity to the vagina . Often described as the “neck” of the womb (from the Latin cervix, meaning neck), this cylindrical structure measures approximately 2.5 to 3.5 centimeters (1 to 1.3 inches) in length .
Anatomical Features
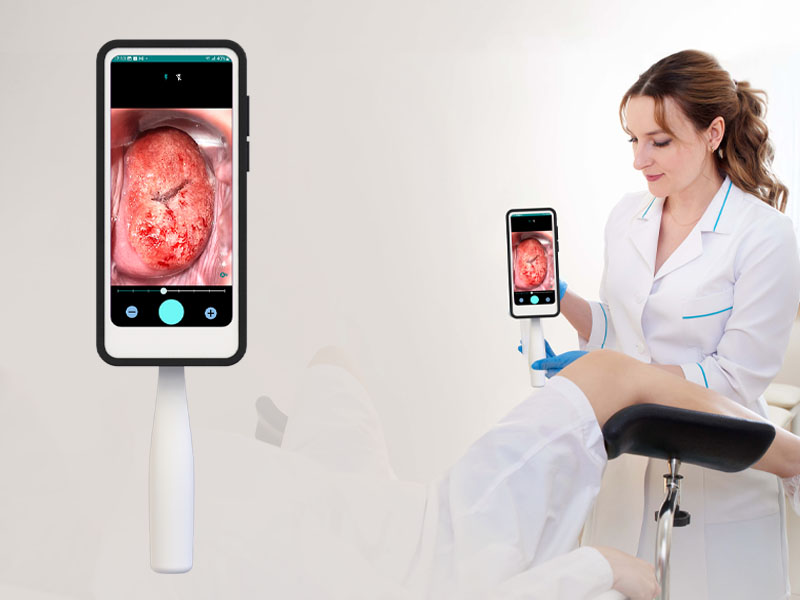
The cervix contains a narrow passage called the cervical canal, which serves two critical functions:
- Menstrual flow: Allows blood from the uterine lining to pass from the uterus into the vagina
- Reproduction: Permits sperm to travel from the vagina upward into the uterine cavity and fallopian tubes for fertilization
- Childbirth: Dilates during labor to allow the baby to pass from the uterus into the birth canal
The cervix is divided into two main regions:
| Region | Description |
|---|---|
| Ectocervix | The portion visible during a pelvic exam, projecting into the vagina |
| Endocervical canal | The passageway through the cervix connecting the uterus to the vagina |
A critical anatomical feature is the transformation zone—the area where the glandular cells of the endocervix meet the squamous cells of the ectocervix. This zone is where most cervical precancers and cancers originate because it is particularly susceptible to HPV infection and cellular changes.
Physiological Functions
Beyond its mechanical roles, the cervix plays an active part in reproductive health:
- Produces cervical mucus that changes in consistency throughout the menstrual cycle to either facilitate or block sperm transport
- Forms a protective barrier against ascending infections from the vagina
- Contains immune cells that help defend against pathogens
Common Conditions Affecting the Cervix
A range of conditions can affect cervical health :
- Cervical intraepithelial neoplasia (CIN) or dysplasia – Precancerous changes in cervical cells
- Cervical cancer – Malignant transformation, most often linked to HPV
- Cervical infections – Including cervicitis from bacterial, viral, or fungal causes
- Cervical polyps – Benign growths on the cervical canal
- Cervical incompetence – Weakness of cervical tissue leading to pregnancy loss
Understanding this anatomy is essential because cervical disease prevention hinges on detecting cellular abnormalities at the transformation zone—long before they progress to invasive cancer.
Part 2: The Disease Spectrum – From Infection to Malignancy
Cervical disease exists on a continuum. The progression from a healthy cervix to invasive cancer follows a well-characterized multistep process that typically unfolds over 12 to 15 years . This slow progression creates an extraordinarily wide window for intervention—if we can detect it.
The Natural History of Cervical Carcinogenesis
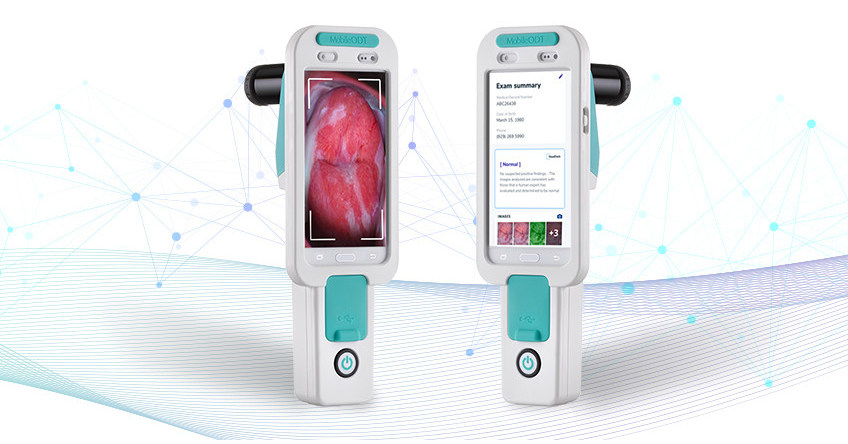
The progression follows a predictable pattern :
1. Acute HPV Infection – Most sexually active individuals will acquire HPV at some point. The immune system clears approximately 90% of HPV infections spontaneously within 1-2 years, with no lasting consequences.
2. Viral Persistence – When the immune system fails to clear the virus, persistent infection with a high-risk HPV genotype (especially HPV16 or HPV18) establishes itself. This is the critical turning point.
3. Low-Grade Squamous Intraepithelial Lesion (LSIL/CIN1) – The virus causes mild cellular abnormalities. At this stage, spontaneous regression remains common, especially in younger women.
4. High-Grade Squamous Intraepithelial Lesion (HSIL/CIN2/3) – Cellular changes become more severe. These lesions have significant potential to progress to cancer if untreated.
5. Invasive Carcinoma – Cancer cells break through the basement membrane and begin invading surrounding tissues.
The Spectrum of Cervical Disease
| Stage | Terminology | Key Features | Prognosis |
|---|---|---|---|
| Healthy | Normal | No cellular abnormalities | — |
| Early infection | Acute HPV | Often asymptomatic, usually clears | Excellent |
| Mild dysplasia | CIN1, LSIL | Mild cellular changes; high regression rate | Usually self-limited |
| Moderate dysplasia | CIN2 | Moderate changes; intermediate risk | Requires treatment |
| Severe dysplasia | CIN3, HSIL | Severe changes; high progression risk | Requires treatment |
| Early cancer | Stage I | Confined to cervix | Treatable with surgery |
| Advanced cancer | Stage II-IV | Spread beyond cervix | Requires multimodal therapy |
Clinical Manifestations
When cervical disease produces symptoms—often only in advanced stages—they may include :
- Abnormal vaginal bleeding (between periods, after intercourse, or after menopause)
- Unusually heavy menstrual periods
- Abnormal vaginal discharge (watery, bloody, or malodorous)
- Pelvic pain or dull backache
- Painful urination or frequent urination
The silent nature of early cervical disease is precisely why screening is so critical—by the time symptoms appear, cancer may already be advanced.
Part 3: The Central Role of HPV Infection
Understanding Human Papillomavirus
Human papillomavirus (HPV) is the necessary cause of cervical cancer. This statement—supported by decades of research and a Nobel Prize to Harald zur Hausen—represents one of the most important discoveries in cancer prevention .
HPV is an extremely common sexually transmitted infection. The Centers for Disease Control and Prevention estimates that most sexually active individuals will contract HPV at some point in their lives. The vast majority of these infections cause no harm and resolve spontaneously.
High-Risk vs. Low-Risk HPV Types
Not all HPV types are created equal:
| Category | HPV Types | Associated Conditions |
|---|---|---|
| High-risk (oncogenic) | 16, 18, 31, 33, 45, 52, 58 | Cervical cancer, other anogenital cancers, oropharyngeal cancer |
| Low-risk (non-oncogenic) | 6, 11 | Genital warts, benign respiratory papillomas |
HPV16 and HPV18 are responsible for approximately 75-80% of all cervical cancer cases . HPV16 alone accounts for more than half of all cervical cancers.
Molecular Mechanisms of HPV-Induced Carcinogenesis
The transformation from a benign viral infection to cancer is driven by viral oncoproteins—specifically E6 and E7—that hijack the cell’s normal regulatory machinery .
The E6 Oncoprotein: Disabling p53
Under normal circumstances, the p53 tumor suppressor protein acts as the cell’s “guardian of the genome.” When DNA damage occurs, p53 either halts cell division to allow repair or triggers programmed cell death (apoptosis).
HPV E6 inactivates p53 by:
- Binding to E6-associated protein (E6AP), an E3 ubiquitin ligase
- Forming a complex that targets p53 for proteasomal degradation
- Eliminating p53 from the cell entirely
Without functional p53, cells with DNA damage continue to divide unchecked, allowing genomic instability to accumulate .
The E7 Oncoprotein: Inactivating pRb
The retinoblastoma protein (pRb) normally controls the cell cycle by binding to E2F transcription factors, preventing them from activating genes required for DNA synthesis.
HPV E7 disrupts this control by:
- Binding to pRb through its conserved LXCXE motif
- Displacing E2F and triggering inappropriate S-phase entry
- Promoting proteasome-mediated degradation of pRb
The combined effect of E6 and E7 is the simultaneous loss of two major tumor suppressor pathways—a powerful driver of malignant transformation .
The E5 Oncoprotein: Supporting Role
While less studied than E6 and E7, the E5 oncoprotein plays an accessory role by:
- Enhancing epidermal growth factor receptor (EGFR) signaling
- Prolonging mitogenic signaling through MAPK and PI3K/AKT pathways
- Reducing antigen presentation, aiding immune evasion
HPV/HIV Co-Infection: A Synergistic Crisis
The interaction between HPV and HIV creates a particularly dangerous situation. HIV-induced immunosuppression—characterized by depletion of CD4+ T lymphocytes—dramatically alters the natural history of HPV infection .
Key effects of HIV co-infection:
- Reduced HPV clearance due to impaired immune surveillance
- Increased persistence of high-risk HPV types
- Higher likelihood of multi-type HPV infections
- Accelerated progression from precancerous lesions to invasive cancer
- Greater risk of treatment failure and recurrence
HIV proteins (Tat, Nef, Vpu, Vif) further amplify oncogenesis by enhancing HPV E6/E7 expression, activating pro-survival pathways (PI3K/Akt, NF-κB), and promoting chronic inflammation .
For women living with HIV, the risk of cervical cancer is substantially elevated, making integrated screening and treatment essential.
Part 4: Traditional Screening – The Pap Smear
History and Principles
The Papanicolaou (Pap) test, developed by Dr. George Papanicolaou in the 1940s, revolutionized cervical cancer prevention. By collecting cells from the cervix and examining them under a microscope for abnormalities, the Pap smear made it possible to detect precancerous changes years before cancer develops.
How Pap Smear Testing Works
The procedure is straightforward:
- A speculum is inserted to visualize the cervix
- A spatula or brush collects cells from the transformation zone
- Cells are spread on a slide (conventional Pap) or suspended in liquid (liquid-based cytology)
- Slides are stained and examined by a cytotechnologist or pathologist
Results are reported using the Bethesda System, which categorizes findings as:
- Negative for intraepithelial lesion or malignancy (NILM) – Normal
- ASC-US – Atypical squamous cells of undetermined significance
- LSIL – Low-grade squamous intraepithelial lesion
- HSIL – High-grade squamous intraepithelial lesion
- ASC-H – Atypical squamous cells, cannot exclude HSIL
- AGC – Atypical glandular cells
- Squamous cell carcinoma or adenocarcinoma
Strengths of the Pap Smear
Traditional cytology has remarkable strengths that have made it the backbone of cervical screening for decades :
| Metric | Performance |
|---|---|
| Sensitivity | 94.5% – Excellent at detecting true disease |
| Negative Predictive Value | 90.3% – Reliable for ruling out disease |
| High-grade lesion detection | 100% concordance with histopathology |
The Pap smear’s high sensitivity means it rarely misses significant disease—a crucial feature for a screening test.
Limitations of Traditional Screening
Despite its successes, the Pap smear has significant limitations that have driven the search for better approaches :
1. Modest Specificity (50.9%) – The test produces many false positives, especially for low-grade abnormalities. In one study, ASC-US showed 55.6% discordance with histopathology, while AGC showed 66.7% discordance .
2. Benign Mimics – Inflammation from cervicitis, recent intercourse, or other benign conditions can produce abnormal-appearing cells, leading to unnecessary follow-up and anxiety.
3. Subjectivity – Cytology interpretation is inherently subjective, with significant inter-observer variability even among expert pathologists.
4. Infrastructure Requirements – Pap testing requires trained cytotechnologists, pathologists, staining reagents, and reliable electricity—resources scarce in many low-resource settings.
5. Single-Time Point – The Pap smear provides only a snapshot of cervical health at the moment of collection.
6. Inability to Detect Glandular Lesions – Adenocarcinomas (cancers of the glandular cells) are more difficult to detect on Pap smears than squamous cell cancers.
The Global Access Problem
The limitations of Pap smear screening are most acute in low- and middle-income countries (LMICs), where only 11% of women aged 30-49 have ever undergone cervical cancer screening, compared to 84% in high-income countries . This disparity directly contributes to the 94% of cervical cancer deaths that occur in LMICs.
Part 5: The Shift Toward Early Diagnostics and Prevention
Changing Paradigms
The limitations of cytology have driven a fundamental shift in cervical screening philosophy: from detecting cellular abnormalities to detecting the virus that causes them.
Modern cervical prevention rests on three pillars:
HPV Testing as Primary Screening
Primary HPV testing—using the test as the initial screening method rather than cytology—offers several advantages:
- Higher sensitivity for detecting high-grade precancerous lesions
- Objective results (molecular, not subjective)
- Longer screening intervals (negative HPV test provides reassurance for 3-5 years)
- Self-collection capability (samples can be collected by the patient herself)
Many countries have now adopted HPV testing as their primary screening modality, with cytology reserved for triage of HPV-positive results.
The WHO Elimination Strategy
In 2020, the World Health Organization launched a global strategy to eliminate cervical cancer as a public health problem. The “90-70-90” targets by 2030 are ambitious but achievable :
| Target | Goal |
|---|---|
| 90% of girls fully vaccinated with HPV vaccine by age 15 | Primary prevention |
| 70% of women screened with a high-performance test by age 35 and again by 45 | Secondary prevention |
| 90% of women with precancer treated and 90% with invasive cancer managed | Tertiary prevention |
Achieving these targets would reduce cervical cancer incidence by 97% and avert 62 million deaths over the next century.
Part 6: Emerging Diagnostics – Biomarkers
The Need for Better Triage
While HPV testing is highly sensitive, it identifies many women with transient infections that will clear spontaneously. Triage tests are needed to distinguish women who need immediate colposcopy from those who can safely be followed with repeat testing.
Non-Coding RNAs as Biomarkers
Recent research has identified non-coding RNAs—including microRNAs (miRNAs), long non-coding RNAs (lncRNAs), and circular RNAs (circRNAs)—as promising biomarkers for cervical cancer detection .
MicroRNAs are small RNA molecules that regulate gene expression. Specific miRNA signatures have been associated with:
- HPV status
- Disease stage
- Risk of progression
- Treatment response
The advantage of RNA-based biomarkers is their ability to reflect active biological processes rather than just viral presence.
Methylation Markers
DNA methylation—the addition of methyl groups to DNA—is an epigenetic change that can silence tumor suppressor genes. Specific methylation patterns in HPV DNA or host genes can distinguish:
- Transient from persistent infection
- Low-grade from high-grade lesions
- Lesions likely to progress from those likely to regress
Methylation-based tests are emerging as powerful triage tools for HPV-positive women.
Protein Biomarkers
p16 and Ki-67 are proteins that can be detected by immunocytochemistry:
- p16 is overexpressed when pRb is inactivated by HPV E7
- Ki-67 marks proliferating cells
Dual staining for p16/Ki-67 on the same slide has shown high specificity for detecting high-grade lesions, reducing unnecessary colposcopies.
Biosensors for Point-of-Care Testing
Biosensor technology is advancing rapidly, with the goal of creating rapid, inexpensive, portable tests for HPV and cervical biomarkers . These devices typically combine:
- Biological recognition elements (antibodies, DNA probes)
- Transducers (electrochemical, optical, or piezoelectric)
- Signal processing electronics
The promise of biosensors is decentralized testing—bringing cervical screening to primary care clinics, pharmacies, and even homes.
Part 7: Artificial Intelligence in Cervical Screening
The AI Revolution in Diagnostics
Artificial intelligence (AI)—particularly machine learning and deep learning—is transforming cervical cancer screening by addressing the fundamental limitation of cytology: human subjectivity .
AI systems can be trained on thousands or millions of cytology images to recognize patterns associated with normal, precancerous, and cancerous cells. Once trained, these systems can:
- Analyze images faster than human experts
- Achieve consistent, reproducible results
- Detect subtle patterns humans might miss
- Operate in settings with limited specialist availability

How AI-Powered Cervical Screening Works
A typical AI-supported cytology workflow includes :
- Sample collection by healthcare worker or patient
- Slide preparation and staining using standard protocols
- Digital scanning to create high-resolution whole-slide images
- AI analysis using cloud-based or on-premise algorithms
- Remote expert verification for quality assurance
The turnaround time for AI analysis can be as short as 10 to 40 minutes—dramatically faster than traditional cytology .
Real-World Implementation: The East Africa Experience
A landmark project implementing AI-supported cervical cancer screening in rural Kenya and Tanzania demonstrates both the promise and challenges of this technology .
The Approach:
- Laboratories established in primary healthcare hospitals
- Existing infrastructure (electricity, water, mobile networks) utilized
- Samples digitized and uploaded to cloud for AI analysis
- Local healthcare workers trained in specimen collection and digital data entry
Successes:
- AI enabled rapid analysis at scale without on-site pathologists
- Multi-disease diagnostic capabilities
- Training center established for regional capacity building
Challenges Encountered:
- Unreliable reagent supply affecting staining quality
- Power interruptions disrupting workflows
- Reagent batch variation causing AI performance degradation
- Limited treatment capacity influencing diagnostic thresholds
Key Lessons for AI Implementation
The East Africa experience reveals critical insights for scaling AI diagnostics :
- Technology must fit local context – Tools designed for high-income settings often fail in low-resource environments
- Infrastructure matters – Offline-capable systems, robust to power fluctuations, are essential
- Supply chain stability – AI performance depends on consistent reagent quality
- Integration over isolation – AI tools cannot succeed without corresponding investment in treatment capacity
- Community engagement – Stigma and mistrust remain barriers regardless of technology
Regulatory and Implementation Barriers
Several interlocking barriers must be addressed for AI diagnostics to achieve their potential :
| Barrier Category | Specific Challenges |
|---|---|
| Health system | Intermittent electricity, limited internet, shortage of trained personnel |
| Regulatory | Unclear approval pathways, data management concerns, privacy issues |
| Financing | Short-term affordability, procurement systems ill-suited for new tech |
| Cultural | Stigma, mistrust of technology, low awareness of screening benefits |
| Technical | Model performance degradation across populations and settings |
Part 8: Microbiome Science and Cervical Health
The Cervical Microbiome
The cervix, like other mucosal surfaces, hosts a community of microorganisms—bacteria, fungi, and viruses—collectively known as the cervicovaginal microbiome. Emerging research suggests that the composition of this microbial community influences susceptibility to HPV persistence and progression.
Lactobacillus Dominance vs. Dysbiosis
A healthy cervicovaginal microbiome is typically dominated by Lactobacillus species (particularly L. crispatus, L. iners, L. gasseri, and L. jensenii), which produce lactic acid and maintain an acidic pH (≤4.5) that inhibits pathogen growth.
Lactobacillus-dominant microbiome → Protective
- Low pH inhibits many pathogens
- Lactic acid has antiviral properties
- Associated with rapid HPV clearance
Diverse, non-Lactobacillus-dominant microbiome (dysbiosis) → Risk factor
- Higher pH (≥4.5)
- Associated with bacterial vaginosis
- Linked to persistent HPV infection
- May promote chronic inflammation
Potential Mechanisms
How might the microbiome influence cervical carcinogenesis?
- Immune modulation – Certain bacteria can alter local immune responses, potentially impairing HPV clearance
- Inflammation – Dysbiotic communities may promote chronic inflammation, a known cancer risk factor
- Metabolite production – Bacterial metabolites may directly affect epithelial cell biology
- Co-infection interactions – Other sexually transmitted infections may interact with HPV
Therapeutic Implications
Understanding the microbiome opens possibilities for novel interventions:
- Probiotics – Restoring Lactobacillus dominance after antibiotic use or dysbiosis
- Prebiotics – Supporting beneficial bacterial growth
- Live biotherapeutics – Engineered bacteria delivering therapeutic molecules
While microbiome-based therapies for cervical disease remain investigational, this represents an exciting frontier in women’s health.
Part 9: At-Home Testing – Empowering Patients
The Self-Sampling Revolution
One of the most transformative developments in cervical screening is the ability for women to collect their own samples for HPV testing . Self-sampling addresses several persistent barriers to screening:
- Privacy and comfort – Many women prefer self-collection to pelvic exams
- Access – Reaches women who cannot or will not visit a clinic
- Resource efficiency – Reduces demand for clinical staff and equipment
- Stigma reduction – Especially important in cultures where gynecologic exams are taboo
How At-Home Cervical Testing Works
Modern at-home HPV testing kits typically include:
- A vaginal swab or cervical brush with clear instructions
- A collection tube with transport medium
- A prepaid mailer for returning the sample to the laboratory
- Secure online portal for receiving results
The laboratory performs molecular HPV testing on the self-collected sample, with results available in 1-2 weeks.
Clinical Performance
Studies have shown that self-collected samples perform comparably to clinician-collected samples for HPV testing. Sensitivity for detecting high-grade cervical lesions is slightly lower than clinician collection but remains acceptable for screening purposes.
Current Options and Availability
As of 2026, several FDA-approved at-home HPV testing options exist in the United States:
- teal Health – First FDA-authorized at-home HPV test (2024)
- Nurx – At-home HPV testing kit with telehealth follow-up
- Everlywell – HPV testing as part of women’s health panel
- LetsGetChecked – At-home STD testing including high-risk HPV
Limitations and Caveats
At-home testing is not without limitations:
- Cannot replace cytology – Self-collected samples are not suitable for Pap smear interpretation
- Follow-up required – Positive results require confirmatory testing and potentially colposcopy
- Sample quality – Improper collection may yield invalid results
- Digital divide – Online result delivery assumes internet access
The Future of At-Home Cervical Health
The next generation of at-home testing may include:
- Integrated HPV + cytology – Devices that preserve cells for both analyses
- Rapid results – Point-of-care tests with results in minutes, not days
- Biomarker panels – Multiple markers (HPV, methylation, proteins) from a single sample
- AI-assisted interpretation – Smartphone-based image analysis of self-collected samples
Part 10: Future Screening Technologies on the Horizon
Integrated Multi-Omics Approaches
The future of cervical screening lies not in any single test but in integrating multiple data streams:
- Genomics – HPV genotype, viral load, integration status
- Epigenomics – DNA methylation patterns
- Transcriptomics – Host and viral gene expression (including non-coding RNAs)
- Proteomics – Protein biomarkers (p16, Ki-67, others)
- Metagenomics – Microbiome composition
- Clinical data – Age, HIV status, vaccination history, previous results
Machine learning algorithms can integrate these diverse data types into a risk score that guides management with greater precision than any single marker.
Point-of-Care Molecular Testing
Technologies are emerging that bring molecular HPV testing to the point of care, eliminating the need for central laboratory processing:
- Isothermal amplification – Detects DNA without thermal cycling (e.g., loop-mediated isothermal amplification, or LAMP)
- Microfluidic cartridges – Self-contained, disposable test cartridges
- Smartphone-connected readers – Portable devices that interpret results
These technologies could make high-performance cervical screening available in primary care clinics, mobile health units, pharmacies, and even homes in low-resource settings.
Liquid Biopsy for Cervical Cancer
The concept of liquid biopsy—detecting cancer signals in blood or other body fluids—is being explored for cervical cancer. Potential applications include:
- Early detection – Identifying cervical cancer before it is clinically apparent
- Treatment monitoring – Tracking response to therapy
- Recurrence surveillance – Detecting residual or recurrent disease
Therapeutic Vaccines
While current HPV vaccines are prophylactic (preventing initial infection), therapeutic vaccines aim to clear established HPV infections and precancerous lesions. Several approaches are in development:
- Peptide vaccines – Targeting HPV E6/E7 proteins
- DNA vaccines – Delivering genes encoding HPV antigens
- Vector-based vaccines – Using modified viruses to deliver HPV antigens
- Cell-based vaccines – Using patients’ own immune cells
Therapeutic vaccines could transform management of HPV-related disease, potentially eliminating the need for excisional procedures.
Conclusion: A Vision for the Future of Cervical Health
The landscape of cervical disease prevention is being fundamentally reshaped by technological innovation. Where the Pap smear served for half a century as the sole screening tool, we now have a diverse toolkit: molecular HPV testing, AI-powered image analysis, biomarker panels, microbiome assessment, and at-home self-sampling.
The implications are profound:
Hidden Biomarkers & Genetic DetectionFor patients – Screening becomes more accessible, less invasive, and more convenient. At-home options respect privacy and autonomy. Positive results come with clearer guidance about risk.
For providers – AI assistance reduces subjective variability and expands reach. Point-of-care tests enable immediate results and same-day management decisions.
For health systems – Self-sampling and automated analysis reduce demands on specialist personnel. Risk-stratified algorithms optimize resource allocation.
For global health – Technologies designed for low-resource settings can finally address the vast disparities in cervical cancer outcomes. The tools to eliminate cervical cancer exist; the challenge is ensuring they reach everyone.
Yet technology alone is insufficient. As the East Africa AI project demonstrated, implementation barriers—reagent supply chains, treatment capacity, community trust—can undermine even the most sophisticated diagnostics . True progress requires concurrent investment in health system strengthening, workforce training, and community engagement.
The goal is ambitious but achievable: a world where no woman dies of cervical cancer. With continued innovation and committed implementation, that future is within reach.
References
- Linder N, Nyirenda D, Mårtensson A, et al. AI supported diagnostic innovations for impact in global women’s health. BMJ. 2025;391:e086009.
- 7612 – Cervix, disease or injury of. Medical EPSS.
- Molecular, immunological and oncogenic mechanisms of cervical cancer mediated by HPV/HIV co-infection. Infectious Agents and Cancer. 2026;21:12.
- Bhagyashree, Rituraj, Pant P, Sharma P. Strengths and Limitations of Pap Smear Screening: When Cytology Succeeds and Where it Fails. OJHAS. 2025;24(2).
- Mousavinejad SN, et al. Cervical cancer diagnostics: non-coding RNAs and biosensors to AI-derived methods. Clin Chim Acta. 2025;120641.
- Cervix. MedlinePlus Medical Encyclopedia.
- Snijders PJF, Steenbergen RDM, Heideman DAM, Meijer CJLM. HPV-mediated cervical carcinogenesis: concepts and clinical implications. J Pathol. 2006;208(2):152-164.
- Strengths and Limitations of Pap Smear Screening. DOAJ.
- Nasretdinova DB. Modern advancements in cervical cancer prevention, early recognition, and prognostic assessment. Central Asian Journal of Medicine. 2025;(3):266-272.
- Cervix. UI Health Care.
⚠️ Medical Disclaimer
The information provided in this content is for educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. While every effort has been made to ensure accuracy and alignment with current clinical standards, medical knowledge and guidelines may evolve over time.
Always seek the guidance of a qualified healthcare provider or gynecologist regarding any questions you may have about cervical health, screening, or symptoms. Never disregard professional medical advice or delay seeking care because of something you have read here.
This content does not establish a doctor–patient relationship and should not be used for self-diagnosis or treatment decisions. If you experience symptoms such as abnormal bleeding, pelvic pain, or unusual discharge, consult a medical professional promptly.