If you have been diagnosed with type 2 diabetes, or if you have noticed strange changes in your feet, you have likely asked a very important question: Why do feet get affected by diabetes more than any other part of the body?
🦶 The Healing Feet Plate
📋 Foot-Smart Reminders
Auto-sliding • Tap or hover to pause • Swipe-friendly
🥗 Healing Feet Foods
- Fatty fish (salmon, sardines)
- Leafy greens & berries
- Nuts, seeds & legumes
- Whole grains & citrus
🚫 Avoid These “Foot Killers”
- Sugary drinks & white bread
- Fried & processed meats
- Full-fat dairy & excess salt
- Alcohol & high-sugar snacks
✅ Daily Foot Do’s
- Wash & dry gently (test water temp)
- Moisturize (not between toes)
- Inspect feet with mirror every night
- Wear clean socks & proper shoes
- Walk 30 min/day & see a podiatrist yearly
⛔ Never-Ever Rules
- No barefoot walking, no heating pads
- No OTC corn removers / razors
- No tight socks, no leg crossing
- No smoking, no ignoring sores >24h
⭐ Tip: After download, you can print or share with family, doctors, or caregivers.
It is a question that haunts millions of Americans. You may have swelling, numbness, pain, or wounds that will not heal. Perhaps you have searched for diabetic feet pictures beginning stages late at night, worried about what you are seeing in the mirror. You are not alone. Over 38 million Americans have diabetes, and nearly half will develop some form of diabetic foot complication in their lifetime.
The answer to “why do feet get affected by diabetes” is surprisingly simple: Your feet are the farthest point from your heart, and they have the smallest blood vessels. High blood sugar damages those tiny vessels and the nerves that run alongside them. The damage shows up in your feet first because they are the “end of the line” for circulation and sensation.
This article will answer every question you have. We will cover why diabetes targets feet (not hands), what early stage diabetes feet look like with pictures described in words, how to recognize woman early signs of diabetic feet, what diabetic foot pain symptoms feel like, how to manage type 2 diabetes feet and type two diabetes swollen feet, and most importantly—how to cure diabetic feet or at least reverse early damage.
Part 1: Why Do Feet Get Affected by Diabetes? (The Core Question)
Let us answer the primary question clearly and directly.
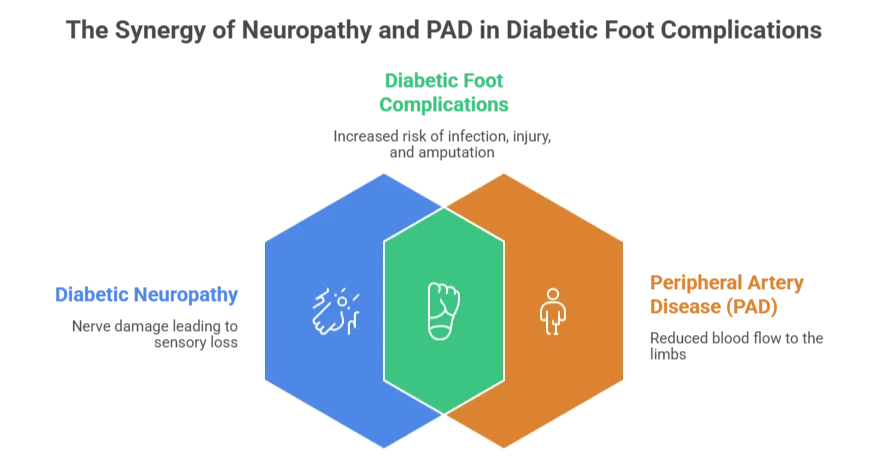
Why do feet get affected by diabetes? The answer involves two medical problems that happen together: diabetic neuropathy (nerve damage) and peripheral artery disease (blood vessel damage).
The Nerve Explanation (Neuropathy)
High blood sugar is toxic to nerves. Over months and years of elevated glucose, the sugar molecules attach to nerve proteins and create inflammatory compounds called advanced glycation end-products (AGEs). These AGEs destroy the myelin sheath—the insulation that allows nerves to send signals quickly.
Your feet have the longest nerves in your body. They run from your spinal cord all the way down to your toes. Because they are so long, they are the most vulnerable. Think of it like a copper wire: a short wire works fine, but a very long wire with damaged insulation will fail at the far end. That far end is your feet.
The Blood Vessel Explanation (Peripheral Artery Disease)
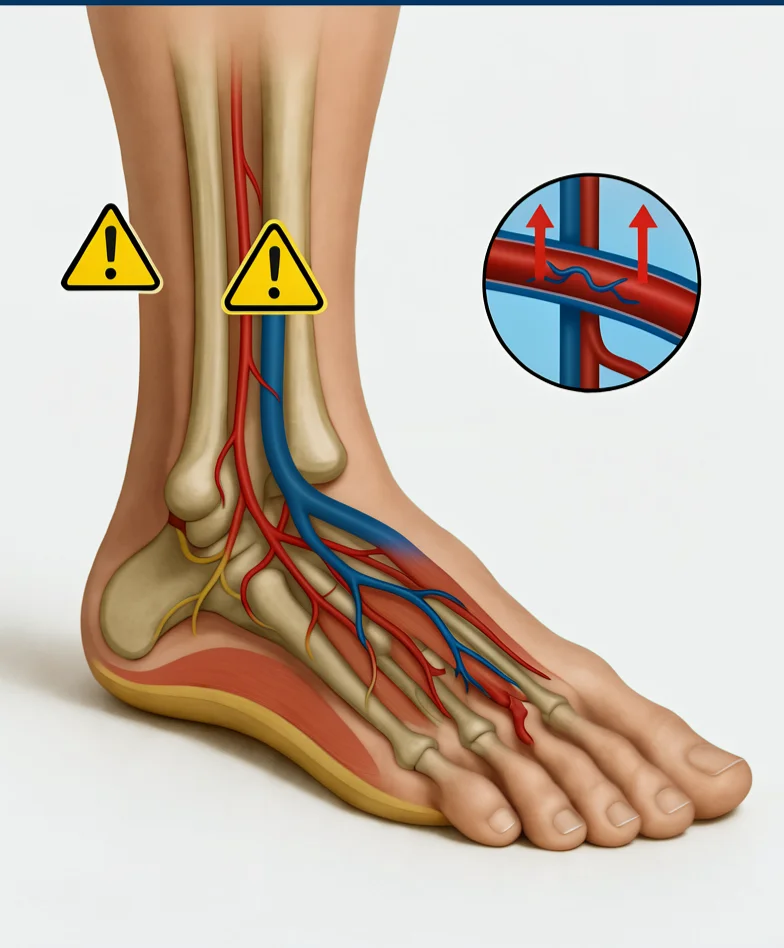
High blood sugar also damages the inner lining of blood vessels (the endothelium). This damage allows cholesterol and fat to stick to vessel walls, causing narrowing and hardening (atherosclerosis). The arteries that feed your feet are small and far from the heart. By the time blood reaches your feet, the pressure has dropped significantly, and any narrowing becomes a crisis.
When you combine numbness (so you do not feel injuries) with poor circulation (so injuries do not heal), a small blister from a tight shoe can become a non-healing ulcer, then infection, then gangrene, then amputation.
Part 2: Why Does Diabetes Affect Feet and Not Hands?
This is an excellent and common question. Many people notice numbness or tingling in their feet years before their hands are affected. Why the difference?
Why does diabetes affect feet and not hands first? Three reasons:
- Distance from the heart: Your feet are farther away than your hands. Gravity also works against blood returning from your feet. Your hands are at heart level most of the day, so circulation is easier.
- Pressure and weight-bearing: Your feet bear your entire body weight every time you stand or walk. Your hands do not. The constant pressure on the soles of your feet compresses tiny blood vessels and nerves, accelerating damage.
- Holding pattern: Your hands move constantly. Movement pumps fluid and blood through tissues. Your feet are often still (sitting, standing, sleeping), which allows inflammatory waste products to accumulate.
That said, advanced diabetes can affect hands. Carpal tunnel syndrome is more common in people with diabetes, and some develop “diabetic cheiroarthropathy” (stiff, waxy hands). But the feet are always affected first and worst.
Part 3: Diabetic Feet Pictures Beginning Stages
You may have searched for diabetic feet pictures beginning stages because you want to compare what you are seeing. While I cannot show actual photos here, I can give you a precise, detailed description of what early stage diabetic feet look like. Use this as your visual guide.
Stage 1: The “At Risk” Foot (No Open Sores Yet)
What you see (described as a picture):
- Dry, flaky, peeling skin, especially on the heels
- Calluses forming on pressure points (ball of the foot, heel, big toe joint)
- Slight redness or warmth over bony areas
- Mild swelling (edema) that comes and goes
- Yellowish, thick, brittle toenails (often fungal)
What you feel: Little or no pain. You may feel “pins and needles” or a vague sense that your feet are “asleep.” Some people describe it as walking on bubble wrap or thick socks.
Stage 2: The “Neuropathic” Foot (Visible Changes)
What you see:
- Loss of the normal arch—the foot becomes flat and wide
- Skin becomes shiny, thin, and hairless (lack of blood flow)
- Toes begin to curl (hammer toes) or drift sideways
- The “rocker bottom” shape may begin (high arch collapses)
- Dark red or purple discoloration when the foot is dangling down
What you feel: Numbness. You cannot feel a pinprick or a light touch. You may not realize your shoes are too tight.
Stage 3: The “Pre-Ulcer” Foot (Danger Zone)
What you see:
- A pre-ulcer appears as a small, hard, corn-like spot that is actually a pocket of dead tissue under the skin
- A blister filled with clear fluid
- A red, hot spot that does not blanch (turn white) when you press it
- Cracked, fissured skin that looks like dry riverbeds
What you feel: Paradoxically, you may feel nothing at the spot itself, but you may have a deep, burning, or aching pain elsewhere in the foot. This is the most deceptive stage.
Stage 4: The Ulcerated Foot (Medical Emergency)
What you see:
- An open sore, usually on the ball of the foot, the bottom of the big toe, or the heel
- The ulcer may be shallow (like a skinned knee) or deep enough to see yellow fat or white tendon
- Surrounding skin is red, swollen, and warm
- Foul-smelling drainage (pus) may be present
What you feel: May be nothing if neuropathy is severe. If circulation is still okay, you may feel sharp, stabbing pain or a deep ache.
If you see any of these features, seek medical care immediately. Do not wait.
Part 4: Woman Early Signs of Diabetic Feet (Specific to Women)
Women often experience diabetic foot signs differently than men. Hormonal changes (menopause, pregnancy), footwear choices (high heels, narrow flats), and differences in fat distribution all play a role.
Woman early signs of diabetic feet that every woman should know:
| Sign | What It Looks/Feels Like | Why It Happens in Women |
|---|---|---|
| Sudden intolerance to heels | You used to wear 2-inch heels all day. Now your feet burn after 20 minutes. | Early neuropathy changes the way your foot bears weight. Heels worsen pressure on the ball of the foot. |
| Cold feet that never warm up | Even with wool socks and a blanket, your toes feel like ice cubes. | Poor circulation (PAD) is more common in postmenopausal women with diabetes. |
| “Burning” sensation at night | A fire-like pain that keeps you awake, often relieved by hanging your feet off the bed. | This is a classic early neuropathy symptom. Women report it more often than men. |
| Swelling that worsens before your period | Feet that fit into shoes perfectly for two weeks suddenly do not fit for one week. | Hormonal fluid retention combined with diabetic edema. |
| Frequent fungal infections between toes | Itchy, cracked, white, soggy skin between the 4th and 5th toes. | Women’s footwear (ballet flats, boots without breathability) traps moisture. |
| Bruises you do not remember getting | Purple or blue marks on the tops or bottoms of your feet. | You have lost protective sensation. You stubbed your foot and never felt it. |
If you are a woman with type 2 diabetes, pay attention to these signs before you develop a full ulcer.
Part 5: Diabetic Foot Pain Symptoms (What Does It Feel Like?)
Not everyone with diabetic feet has pain. About 50% of people with diabetic neuropathy have no pain at all—only numbness. The other 50% have one or more of the following diabetic foot pain symptoms.
The Six Types of Diabetic Foot Pain
- Burning pain: A hot, sunburn-like sensation on the soles or tops of the feet. Often worse at night.
- Electrical or shock-like pain: Sudden, sharp jolts that feel like a rubber band snapping or a static shock. These last only seconds but can be intense.
- Aching or throbbing pain: A deep, dull ache that feels like a toothache in your foot. Often related to poor circulation rather than nerves.
- Allodynia (pain from light touch): The weight of a bedsheet or the brush of a pant leg feels painful. This is a sign of irritated, angry nerves.
- Cramping pain in the calves (claudication): A tight, squeezing, charley-horse pain in your calves when you walk that goes away with rest. This is not nerve pain—it is vascular pain from peripheral artery disease.
- Rest pain: Pain in the toes or front of the foot that wakes you up at night and improves when you dangle your foot off the bed. This is a sign of critical limb ischemia (severe PAD).
Important: You can have pain AND numbness at the same time. The numbness means you cannot feel cuts or blisters, but you can still feel deep burning or aching. This is a very confusing but dangerous combination.
Part 6: Early Stage Diabetes Feet (The First Changes)
What do early stage diabetes feet look like before any pain starts? Most people miss these signs entirely because they are subtle and come on slowly over years.
The Earliest Changes (Reversible Stage)
- Loss of the ankle reflex: Your doctor checks this by tapping your Achilles tendon. In early diabetes, the reflex becomes sluggish or absent.
- Decreased vibration sense: You cannot feel a tuning fork buzzing on your big toe, even though you can feel it on your shin.
- Abnormal monofilament test: A single nylon fiber (the thickness of a fishing line) bent against your foot feels like a touch, not a poke.
- Decreased sweat production: The skin on your feet becomes dry and cracked because the nerves that control sweating are damaged.
- Toes that do not spread: When you stand barefoot, your toes stay close together rather than naturally splaying for balance.
If you catch early stage diabetes feet at this point, you can often reverse or halt progression with strict blood sugar control, diet change, and proper footwear.
Part 7: Type 2 Diabetes Feet (Specific Risks)
Type 2 diabetes feet are different from type 1 diabetes feet. Type 2 usually develops later in life (after age 45), often alongside obesity, high blood pressure, and high cholesterol. This means the feet are attacked by multiple problems at once.
The “Metabolic Syndrome Foot”
In type 2 diabetes, the feet suffer from:
- Neuropathy (from high blood sugar)
- Peripheral artery disease (from high cholesterol and high blood pressure)
- Obesity-related pressure (excess body weight multiplies force on the soles)
- Slow wound healing (from all of the above)
The result: A person with type 2 diabetes has a 15% lifetime risk of developing a foot ulcer. Once an ulcer develops, the risk of amputation rises to 20-30%.
Type 2 Diabetes Feet Warning Signs (By Age)
| Age Group | Most Common Foot Problem |
|---|---|
| 45-55 | Burning pain at night, cold feet, thick toenails |
| 55-65 | Hammer toes, loss of arch, first ulcers on the ball of the foot |
| 65-75 | Non-healing ulcers, Charcot foot (collapsed arch), gangrene of toes |
| 75+ | Amputation risk highest; falls due to numb feet |
Part 8: Type Two Diabetes Swollen Feet (Edema)
Type two diabetes swollen feet is an extremely common complaint. You may wake up with normal-sized feet but by evening, your shoes feel two sizes too small. Or you press your thumb into your shin and a dent (pit) remains for several seconds.
Why Does Type 2 Diabetes Cause Swollen Feet?
- Poor circulation: Fluid leaks out of damaged blood vessels into the surrounding tissue.
- Heart failure: Many people with type 2 diabetes also have undiagnosed heart failure. When the heart pumps weakly, fluid backs up into the feet.
- Kidney disease (nephropathy): Diabetes is the leading cause of kidney failure. Damaged kidneys cannot filter excess fluid, which settles in the feet.
- Medications: Common diabetes drugs (insulin, thiazolidinediones like pioglitazone) and blood pressure drugs (calcium channel blockers) cause swelling.
- Venous insufficiency: The one-way valves in leg veins fail, allowing blood to pool in the feet.
What to Do About Type Two Diabetes Swollen Feet
- Do not reduce your water intake (dehydration worsens swelling).
- Do elevate your feet above heart level for 30 minutes, three times per day.
- Do wear compression socks (20-30 mmHg gradient) if your arteries are open (your doctor must check your foot pulses first).
- Do reduce sodium intake to less than 1,500 mg per day.
- Do ask your doctor if a diuretic (water pill) is right for you.
When swollen feet are an emergency: If only one foot is swollen (not both), if the swelling is sudden (over hours), or if the swollen foot is hot, red, and painful—go to the emergency room. This could be a blood clot (deep vein thrombosis).
Part 9: How to Cure Diabetic Feet (Realistic Answers)
The question “how to cure diabetic feet” is one of the most searched phrases. Let me be honest with you.
Can you fully cure established diabetic neuropathy? No. Once a nerve is dead, it does not regenerate. Can you reverse early stage diabetes feet? Yes. If you catch the changes before ulcers form, you can stop progression, restore some sensation, and heal the skin.
The “Cure” Protocol (For Early Stage)
This is the closest thing to a cure for diabetic feet. It requires six months of strict discipline.
| Intervention | How to Do It | Expected Result |
|---|---|---|
| Strict blood glucose control | Keep A1C below 7.0% (or as low as safely possible without hypoglycemia) | Reduces further nerve damage. Some small nerve fibers can regrow over 6-12 months. |
| Therapeutic footwear | Custom-molded diabetic shoes or extra-depth shoes with soft insoles | Eliminates pressure points that cause ulcers. Heals pre-ulcerative lesions. |
| Daily foot inspection + moisturizing | 10 minutes every night with a mirror | Catches problems at the pre-ulcer stage. Heals cracked skin. |
| Neuropathy-specific supplements | Alpha-lipoic acid (600 mg/day), benfotiamine (300 mg/day), methylcobalamin (vitamin B12, 1,000 mcg/day) | Reduces burning pain and may support nerve repair. (Ask your doctor first.) |
| Walking program | 30 minutes of daily walking (not standing) in good shoes | Improves circulation. Builds collateral blood vessels around blocked arteries. |
| Smoking cessation | Use nicotine replacement therapy, support groups, or prescription meds (Chantix) | Smoking is the single biggest reversible risk factor. Quitting can restore some blood flow within weeks. |
When Surgery Is the “Cure”
For advanced diabetic feet with blocked arteries, the cure is revascularization:
- Angioplasty and stenting: A balloon opens the narrowed leg artery, and a wire mesh tube (stent) holds it open.
- Bypass surgery: A vein or synthetic tube is sewn around the blocked artery.
These procedures restore blood flow. With good blood flow, ulcers can heal, and amputation can be avoided. This is as close to a cure as modern medicine offers for severe diabetic feet.
Part 10: The Complete Do’s and Don’ts for Diabetic Feet (USA Edition)
The Daily “Do” Checklist
- Do wash feet daily with lukewarm water and mild soap. Test the water with your elbow.
- Do dry thoroughly, especially between the toes.
- Do moisturize the tops and bottoms (not between toes).
- Do inspect every part of both feet using a mirror.
- Do wear clean, seamless, moisture-wicking socks (cotton or diabetic-specific).
- Do wear properly fitted shoes with a wide toe box and soft leather upper.
- Do shake out your shoes before putting them on.
- Do rotate your shoes (wear a different pair each day).
- Do walk for 30 minutes daily (after checking with your doctor).
- Do see a podiatrist at least once per year.
The “Never” Don’t List
- Never walk barefoot (even indoors).
- Never use heating pads, hot water bottles, or electric blankets on your feet.
- Never soak your feet (prolonged soaking dries skin).
- Never use over-the-counter corn, callus, or wart removers (they contain acid).
- Never cut your own calluses or use a razor blade on your feet.
- Never wear socks with tight elastic bands.
- Never cross your legs when sitting.
- Never smoke (any amount).
- Never ignore a cut or sore for more than 24 hours.
Part 11: The Diabetic Foot Diet (What to Eat and Avoid)
To heal your feet from the inside out, you need an anti-inflammatory, low-glycemic, vascular-friendly diet.
Foods to Eat (The “Healing Feet” Plate)
- Fatty fish (salmon, sardines, mackerel): Omega-3s improve blood flow.
- Leafy greens (spinach, kale, collards): Vitamin K keeps arteries flexible.
- Berries (blueberries, blackberries, strawberries): Antioxidants reduce nerve inflammation.
- Nuts and seeds (walnuts, flaxseeds, chia seeds): Magnesium for nerve function.
- Legumes (lentils, chickpeas, black beans): Fiber stabilizes blood sugar.
- Whole grains (oats, quinoa, brown rice): Slow-release energy and B vitamins.
- Citrus (oranges, grapefruit, lemons): Vitamin C strengthens foot skin.
Foods to Avoid (The “Foot Killers”)
| Avoid This | Because |
|---|---|
| Sugary sodas, sweet tea, fruit juice | Cause rapid blood sugar spikes that damage nerves within hours |
| White bread, white rice, pastries, bagels | Act like sugar in the bloodstream |
| Fried foods (fries, donuts, fried chicken) | Trans fats stiffen arteries to the feet |
| Processed meats (bacon, sausage, hot dogs, deli meats) | High sodium causes swelling; nitrates damage vessels |
| Full-fat dairy (whole milk, cheese, butter) | Saturated fats accelerate atherosclerosis |
| Excess alcohol | Blocks B12 absorption (critical for nerves) |
Part 12: When to See a Doctor (The Red Flags)
Seek medical attention immediately if you have:
- A cut, blister, or sore that has not healed after 48 hours
- Redness, warmth, or swelling spreading up the foot or ankle
- A black or dark purple area on any toe or the heel
- Foul-smelling drainage from a wound
- Sudden, severe swelling in one foot only
- Fever with no other explanation plus a foot problem
- Rest pain (pain at night that improves when dangling the foot)
Do not wait for your next scheduled appointment. Go to an urgent care, a podiatrist, or an emergency room.
Final Summary: Your Diabetic Feet Action Plan
- Why do feet get affected by diabetes? Because they have the longest nerves and smallest blood vessels, making them the first to fail when blood sugar is high.
- Early stage diabetes feet show dry skin, calluses, numbness, and loss of arch.
- Woman early signs of diabetic feet include burning night pain, cold feet, and sudden intolerance to heels.
- Diabetic foot pain symptoms range from burning and electrical shocks to deep aching and calf cramps.
- Type two diabetes swollen feet require elevation, compression (if safe), and low sodium.
- How to cure diabetic feet in early stage: Strict glucose control, proper shoes, daily inspection, supplements, and walking.
- The do’s and don’ts are your daily armor. Follow them every single day.
Your feet are not expendable. With the right knowledge and daily habits, you can keep them healthy, pain-free, and mobile for decades. Start today.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Every person with diabetes should have an individualized care plan developed with their primary care physician, endocrinologist, and podiatrist. The dietary and supplement recommendations should be discussed with your doctor before implementation.
References (Selected):
- American Diabetes Association. “Standards of Care in Diabetes—2025.” Diabetes Care.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). “Diabetic Neuropathy.”
- Mayo Clinic. “Diabetic Foot Care: 10 Do’s and Don’ts.”
- Centers for Disease Control and Prevention (CDC). “Diabetes and Your Feet.”
- American Podiatric Medical Association. “Diabetic Foot Wound Care Guidelines.”