Diabetic foot ulcers are one of the most serious and overlooked complications of diabetes, often beginning with minor numbness, dry skin, or unnoticed cuts that gradually develop into deep, infected wounds and know how to treat diabetic foot ulcer at home
Without early detection and proper care, these ulcers can lead to severe infections, hospitalization, and even amputation. Understanding how diabetic foot ulcers are prevented, diagnosed, and medically classified is essential for reducing long-term complications and improving recovery outcomes.
This guide explains the early warning signs, modern diagnostic methods, risk assessment tools, and widely used ulcer classification systems that help doctors determine severity and choose the most effective treatment plan.
Why Prevention Matters
Diabetes increases the risk of foot ulcers due to neuropathy (loss of protective sensation), poor circulation (peripheral artery disease), and impaired healing from high blood sugar. In the USA, DFUs are a major cause of lower-limb amputations, but up to 85% are preventable with consistent care, early detection, and proper management.
According to the American Diabetes Association (ADA) 2026 Standards of Care, annual comprehensive foot evaluations and daily self-care are key to identifying risks and preventing ulcers.
Know Your Risk Level
A podiatrist or diabetes care team should perform regular assessments (at least annually, more often if high-risk). Key risk factors include:
- Loss of protective sensation (tested with 10g monofilament)
- Foot deformities (bunions, hammertoes, Charcot foot)
- History of previous ulcer or amputation
- Poor circulation
- Callus formation
- Poor glycemic control
- Smoking, obesity, or kidney disease
High-risk individuals benefit most from therapeutic footwear and frequent professional care.
Daily Prevention Routine (The Foundation)
- Inspect Your Feet Every Day Check tops, bottoms, sides, heels, and between toes for cuts, blisters, redness, swelling, warmth, calluses, or color changes. Use a mirror or ask for help if needed. Do this consistently — even small issues can escalate quickly without sensation.
- Wash and Dry Properly Wash daily with lukewarm (not hot) water and mild soap. Pat dry thoroughly, especially between toes. Test water temperature with your elbow.
- Moisturize Smartly Apply lotion or cream to tops and bottoms of feet to prevent cracking, but skip between the toes to avoid fungal growth. Urea-based creams are often recommended.
- Nail Care Trim nails straight across after bathing. File edges smooth. If you have neuropathy, poor vision, or thick nails, let a podiatrist handle it.
- Temperature Awareness Avoid hot water, heating pads, or hot soaks — burns can go unnoticed.
Footwear and Protection – Critical for Prevention
- Never go barefoot — even indoors.
- Wear well-fitting, cushioned shoes with a wide toe box and seamless interiors. Check inside shoes daily for objects.
- Use moisture-wicking, seamless socks (light-colored to spot issues easily).
- Therapeutic/Diabetic Shoes: Medicare Part B and many private plans cover them for qualifying high-risk patients (1 pair + inserts per year). They reduce pressure and prevent ulcers. Discuss certification with your doctor.
ADA Recommendation: Specialized therapeutic footwear for those at high risk (neuropathy with callus, deformity, poor circulation, prior ulcer/amputation).
Blood Sugar and Lifestyle Management
- Maintain target blood glucose and HbA1c levels — this improves circulation, nerve health, and healing.
- Follow a balanced diabetes-friendly diet, stay active (with doctor-approved low-impact exercise), and manage weight.
- Quit smoking — it severely impairs blood flow.
- Control blood pressure and cholesterol.
Professional Care and Monitoring
- Annual (or more frequent) comprehensive foot exams — including monofilament testing, vibration sense, and vascular checks.
- Regular podiatrist visits for nail care, callus debridement, and custom offloading if needed.
- Emerging tools (per 2026 ADA updates): Consider temperature-monitoring devices (smart mats, insoles, or socks) for high-risk patients to detect early inflammation.
What to Do for Prevention
- Control diabetes comprehensively.
- Wear proper footwear at all times.
- Perform daily inspections and basic care.
- Address pre-ulcerative signs (calluses, corns, dry skin) promptly with professionals.
- Elevate feet when sitting to improve circulation.
- Stay up-to-date with vaccinations (e.g., flu, pneumonia) to reduce infection risks.
What Not to Do (Common Mistakes)
- Do not ignore any foot changes, even if painless.
- Avoid self-treating corns, calluses, or ingrown nails.
- Never use medicated corn removers or attempt “bathroom surgery.”
- Do not soak feet for long periods.
- Avoid tight shoes, high heels, or pointed toes.
- Do not smoke or use tobacco products.
- Skip going barefoot or wearing worn-out shoes.
Additional Advanced Prevention Tips
- For those in remission after a prior ulcer: Structured education, therapeutic footwear, regular podiatric care, and possible temperature self-monitoring.
- Multidisciplinary care (podiatrist + vascular specialist + diabetes educator) for high-risk cases.
- Offloading techniques (special inserts, braces) if deformities are present.
When to Seek Immediate Help (Red Flags)
Contact your doctor or podiatrist the same day for:
- Any new cut, blister, redness, warmth, or swelling
- Non-healing sore
- Signs of infection (pus, increasing pain, fever)
- Sudden changes in foot shape or temperature
Foot Ulcer Treatment at Home
Mild foot ulcers should always be evaluated by a healthcare professional, especially in people with diabetes. However, proper home care can help support healing and prevent infection from worsening. Basic home treatment includes cleaning the wound gently with saline or clean water, applying a sterile dressing, keeping pressure off the affected foot, and monitoring for redness, swelling, pus, or foul smell. Walking barefoot should be avoided because it increases the risk of deeper injury and infection.
Foot Ulcer Treatment Cream
Doctors may recommend wound-healing creams, moisture-balancing gels, or antibiotic creams depending on the ulcer type and infection risk. Commonly used options include silver-based creams, mupirocin ointment, and specialized diabetic wound dressings that help maintain a moist healing environment. The best cream depends on whether the ulcer is infected, dry, or producing drainage.
Natural Home Remedies for Diabetic Wounds
Natural remedies should never replace medical treatment for serious diabetic ulcers, but some supportive measures may help healing:
- Keeping blood sugar levels controlled
- Eating enough protein and vitamins
- Using honey-based medical dressings approved for wounds
- Staying hydrated
- Avoiding smoking and alcohol
- Keeping pressure off the ulcer
Home remedies should not include harsh chemicals, toothpaste, hydrogen peroxide, or unapproved herbal pastes because these can damage tissue and slow healing.
Diabetic Foot Ulcer Treatment
Treatment for diabetic foot ulcers focuses on:
- Controlling infection
- Improving blood circulation
- Removing dead tissue (debridement)
- Reducing pressure on the foot
- Maintaining blood sugar control
- Using specialized dressings or medications
Severe ulcers may require hospitalization, IV antibiotics, vascular procedures, or surgery if bone infection or gangrene develops.
How to Heal Diabetic Wounds Faster
Diabetic wounds heal faster when:
- Blood sugar remains stable
- The wound stays clean and covered
- Pressure is removed using diabetic footwear or offloading devices
- Infection is treated early
- Proper nutrition supports tissue repair
- Smoking is avoided
Daily wound inspection is critical because diabetic neuropathy may prevent patients from feeling worsening damage.
Non Diabetic Foot Ulcer Treatment
Non-diabetic foot ulcers may develop from poor circulation, pressure injuries, vein disease, trauma, or autoimmune conditions. Treatment usually includes:
- Cleaning and dressing the wound
- Treating the underlying cause
- Compression therapy for venous ulcers
- Antibiotics if infected
- Pressure relief and supportive footwear
Unlike diabetic ulcers, some non-diabetic ulcers heal more quickly if circulation is normal.
Diabetic Foot Ulcer Treatment Medication
Medications commonly used include:
- Oral or IV antibiotics for infection
- Pain medications if needed
- Blood sugar control medications or insulin
- Topical antimicrobial dressings
- Medications that improve blood flow in selected patients
Doctors may also use advanced biologic dressings or growth-factor therapies in chronic wounds.
Best Antibiotic Cream for Diabetic Foot Ulcer
The best antibiotic cream depends on the type of bacteria and wound severity. Commonly prescribed options include:
- Mupirocin ointment
- Silver sulfadiazine cream
- Fusidic acid cream
- Bacitracin-based topical antibiotics
These should only be used under medical guidance because unnecessary antibiotic use can worsen resistance or irritate the wound.
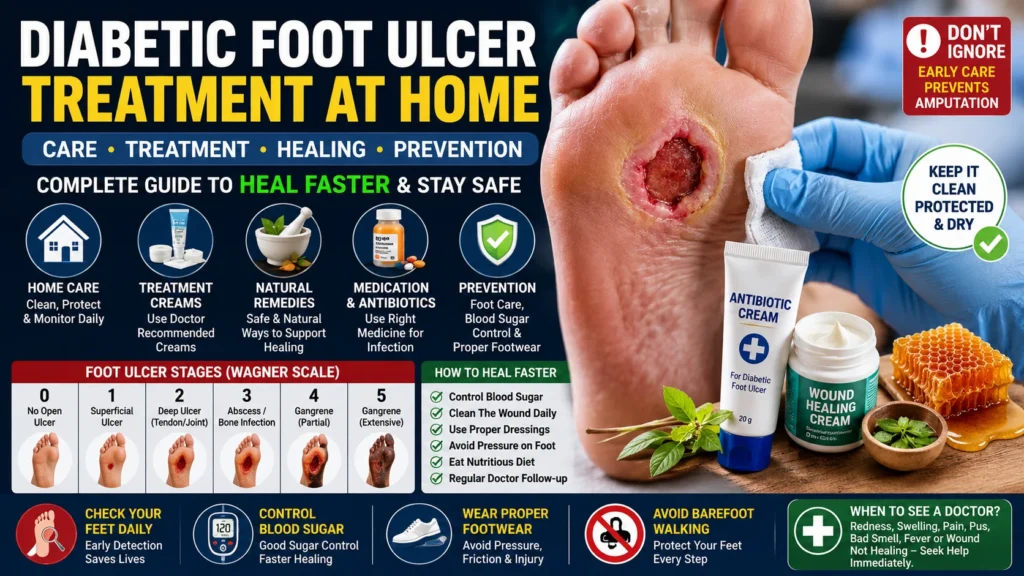
Foot Ulcer Stages Pictures
Diabetic foot ulcers are commonly classified using the Wagner Scale:
- Grade 0: High-risk foot without open wound
- Grade 1: Superficial skin ulcer
- Grade 2: Deep ulcer reaching tendons or joints
- Grade 3: Bone infection or abscess
- Grade 4: Localized gangrene
- Grade 5: Extensive gangrene requiring major amputation
Pictures of ulcer stages help patients recognize early warning signs before severe tissue damage occurs.
FAQS:
1. Can a diabetic foot ulcer heal without surgery if treated early at home?
Yes, many mild diabetic foot ulcers can heal without surgery if they are detected early and treated properly. Successful healing usually depends on keeping blood sugar under control, cleaning the wound daily, using proper dressings, avoiding pressure on the foot, and treating infection quickly. However, deep ulcers, severe infections, poor blood circulation, or bone involvement may require surgical treatment or hospitalization.
2. What does a diabetic foot ulcer look like before it becomes infected?
Before infection develops, a diabetic foot ulcer may appear as a small red sore, blister, crack, or shallow open wound on the foot or toes. The surrounding skin may look dry, callused, or swollen. Some ulcers drain clear fluid or develop a dark edge due to poor circulation. Because diabetic neuropathy reduces sensation, many patients do not feel pain even when tissue damage is progressing.
3. Why do some diabetic foot wounds heal slowly even after using antibiotic creams?
Antibiotic creams alone cannot fix the underlying problems that slow diabetic wound healing. High blood sugar damages blood vessels and nerves, reducing oxygen and nutrient delivery to the wound. Poor circulation, repeated pressure on the foot, smoking, infection, kidney disease, and inadequate nutrition can also delay healing. In many cases, wound care, pressure relief, blood sugar control, and improved circulation are just as important as antibiotics.
Final Thoughts
Preventing diabetic foot ulcers is achievable through daily vigilance, proper footwear, excellent diabetes control, and teamwork with your healthcare providers. Most amputations are preventable when these habits become routine.
Take action today — schedule a foot exam if overdue, discuss therapeutic shoes with your doctor, and commit to daily checks. Your feet will thank you with better mobility and independence for years to come.
Key Sources: American Diabetes Association Standards of Care 2026, IWGDF Guidelines, Medicare guidelines, and CDC/ADA foot care resources.
Would you like a printable daily foot care checklist, more details on therapeutic shoes, or information on temperature-monitoring devices?
Important Disclaimer: This information is for educational purposes only and is not a substitute for professional medical advice. Diabetic foot ulcers (DFUs) can lead to serious infections, hospitalizations, and amputations. Work closely with your healthcare team—including your primary doctor, endocrinologist, and podiatrist—for personalized risk assessment and care. Guidelines evolve; always follow the latest recommendations from your providers.