It often starts without a tremor. There is no dramatic fall, no sudden loss of speech. Instead, for hundreds of thousands of Americans, the story of Parkinson’s disease begins with a series of subtle, frustratingly small changes hidden inside the rhythm of daily life, identify Early Parkinson’s Signs Hidden in Everyday Activities.
For Abby, a musician and avid hiker, the first clue was not a shaking hand but a loss of musical expression. Sitting with her cello, she realized she could no longer produce “vibrato”—the beautiful wavering of pitch that gives a note its emotional weight. She blamed it on a lack of practice after the COVID lockdowns. Simultaneously, her left foot began acting strangely during long charity walks. She chalked it up to the mileage .
👟 Early Parkinson’s Signs
Subtle changes in daily activities · What families & caregivers should watch for
For Veronica Brown, a former travel agent, the prodromal (or pre-diagnosis) stage manifested not as a movement issue but as debilitating anxiety, chronic fatigue, and depression. She stopped traveling. She stopped living the life she loved. It took years before a tremor in her foot finally gave a name to her suffering: young-onset Parkinson’s disease .
These are not isolated incidents. They are the reality of how Parkinson’s disease—the fastest-growing neurodegenerative disease in the world—often begins . We tend to visualize Parkinson’s as a resting tremor, a hunched posture, or a shuffling walk. However, by the time these classic motor symptoms appear, the brain has often already lost more than half of the dopamine-producing neurons in the substantia nigra .
The key to earlier diagnosis—and potentially earlier intervention—lies in recognizing the Early Parkinson’s Signs Hidden in Everyday Activities.
Here is how to spot them in the margins of your day.
The Silent Decade: When the Brain Changes Before You Do
Before we look at the signs, it is crucial to understand the timeline. Parkinson’s is not an overnight invader. It is a slow breakdown of the neurological system. The protein alpha-synuclein begins to misfold and clump together years, sometimes decades, before a clinical diagnosis .
This “prodromal” period is where the disease hides. During this time, the brain is struggling to maintain dopamine levels, but the body is compensating. Eventually, the compensation fails, and the “hidden” signs become apparent—though they are rarely recognized for what they are. According to Parkinson’s Australia, these early symptoms can significantly impact daily life, arising years before the more recognizable motor issues .
To catch them, we need to stop looking for trembling hands and start looking at the quality of our daily actions.
1. The Keyboard Clue: Micrographia and the Loss of Fine Motor Control
One of the most telling early signs happens at the edge of a desk. If you are a writer, a note-taker, or someone who still writes checks, look at your handwriting.
The Hidden Sign: A progressive reduction in the size of your letters, known as micrographia. The writing may appear cramped, the words crowd together on the line, and the spaces between letters shrink. You might write a sentence that starts at a normal size, but by the end, the letters are half the height they were at the start .
Why it happens: Dopamine depletion affects the fine motor control required for precise finger movement. The brain struggles to regulate the force of the muscles, leading to smaller, tighter movements.
Real-world example: Think about filling out a deposit slip at a bank. Where you used to write clearly, you now find your signature looks squished, or you run out of room because the letters didn’t expand as you intended. Many people dismiss this as arthritis or “getting old,” but if the handwriting isn’t shaky—just small—it’s a neurological red flag .
2. The Sleep Battleground: Acting Out Your Dreams (RBD)
This is perhaps the strongest predictor of future Parkinson’s. While many people talk in their sleep or have nightmares, REM Sleep Behavior Disorder (RBD) is different.
The Hidden Sign: Normally, during REM (dream) sleep, your brain sends a signal to paralyze your body. You are essentially “stuck” in a sleeping bag of your own flesh so you don’t hurt yourself while dreaming. In RBD, that paralysis fails. A person will physically act out their dreams. This might involve punching the pillow, kicking a bed partner, yelling, grabbing, or even leaping out of bed .
The Statistics: This is not a quirk. Studies cited by Parkinson’s Australia show that people with idiopathic RBD have a 50% to 80% likelihood of developing Parkinson’s or a similar disorder later in life .
Real-world example: A spouse reports that their partner, who is usually gentle, has started flailing their arms violently during the night, often shouting about being chased or attacked. They wake up with scratches or bruises they don’t remember getting. While not everyone with RBD gets Parkinson’s, this symptom warrants an immediate neurological workup, as it often precedes motor symptoms by 5 to 15 years.
3. The Diner Test: Loss of Smell (Anosmia/Hyposmia)
Have you stopped smelling your coffee brewing in the morning? Can you no longer detect the sharp scent of dill pickles or the distinct sweet smell of licorice? You might think your nose is just stuffy, but the issue might be deeper in the brain .
The Hidden Sign: A diminished ability to detect specific odors, particularly bananas, dill pickles, and licorice, is a known early marker . This isn’t about a stuffy nose due to a cold; it is a neurological inability to process scent.
Why it happens: The olfactory bulb (the brain’s smell center) is often one of the first areas hit by the misfolded proteins that cause Parkinson’s. This symptom can appear 5 to 10 years before any movement issues .
Real-world example: You are cooking dinner and accidentally burn the onions. The smoke detector goes off, but you didn’t smell the smoke. Or, you find yourself putting extra hot sauce and salt on food because everything tastes “bland,” even when dining at a restaurant you used to love.
4. The Quiet Voice: Hypophonia
Communication is an everyday activity that relies on a complex symphony of muscles. In early Parkinson’s, the volume knob gets turned down.
The Hidden Sign: Hypophonia, or soft speech. The person speaks in a low, monotone voice that forces others to ask them to repeat themselves constantly. They may feel like they are shouting, but to the outside world, they sound like they are mumbling .
The Statistic: The Parkinson’s Foundation notes that 89% of people with Parkinson’s experience speech disorders, often beginning with a reduction in volume .
Real-world example: You are at a family dinner. Your loved one tells a story, but everyone at the table has to lean in to hear. They finish, and you realize that the melody of their voice is gone; there is no rise and fall in pitch. It sounds flat and tired.
5. The “Lazy Arm” During Walking
Walking is something we do thousands of times a day, and we rarely think about the mechanics of it—specifically, the swing of our arms.
The Hidden Sign: A reduction or absence of arm swing on one side of the body while walking. The other arm swings normally, but one arm hangs stiffly at the side, almost like it is in a cast .
Why it happens: Walking is an automatic process. When we stride with our right leg, our left arm naturally swings forward to counterbalance the weight. This automatic “pendulum” motion is regulated by the basal ganglia. As dopamine drops, the pendulum stops on one side.
Real-world example: While power walking through the mall, you catch your reflection in a store window. One arm is pumping naturally, but the other looks stiff and stationary. If you try to consciously swing it, you feel awkward and mechanical, not fluid.
6. The Stiff Shoulder (That Won’t Heal)
Pain, specifically musculoskeletal pain, is one of the most frequently missed early symptoms. Patients often bounce between orthopedists and physical therapists for years before landing in a neurologist’s office.
The Hidden Sign: Persistent stiffness or pain in one shoulder, hip, or the back of the neck. Unlike an injury, this stiffness doesn’t go away with rest or standard stretching. It often feels like a “frozen shoulder” that resists movement .
Real-world example: You are a golfer, or a tennis player, and you notice your left shoulder feels “tight” all the time. You stop playing for two weeks, but the moment you pick up the club again, the extreme stiffness returns, limiting your backswing. Because the rigidity of Parkinson’s is constant (it feels like moving through molasses), it mimics a pulled muscle that never heals.
The New Frontier: Your Daily Step Count
In a fascinating development for 2025/2026, researchers are realizing that even the data from your smartwatch or phone might hold hidden clues. A large study published in npj Parkinson’s Disease analyzed step counts from over 95,000 people.
The research found that people who later developed Parkinson’s had lower daily step counts years before their diagnosis. Specifically, people walking more than 12,369 steps per day had a 59% lower risk compared to those walking fewer than 6,276 steps .
Crucially, the study noted that this likely isn’t because walking prevents Parkinson’s, but because the disease slows you down from the inside out long before you notice it. Your step count reflects a subtle, gradual loss of energy and automatic movement .
Parkinson’s is a marathon, not a sprint. By learning to read the subtle signs hidden in your morning writing, your nightly sleep, and your daily walk, you can trade fear for action. You can trade uncertainty for a plan.
Reading this list can be frightening, especially because many of these symptoms—constipation, fatigue, a stiff shoulder—are common to millions of Americans who do not have Parkinson’s. The difference lies in the pattern.
You should speak with a primary care physician or a neurologist if you notice multiple of these symptoms stacking up, particularly if they are one-sided (happening only on the left or only on the right) or if they involve REM sleep behavior disorder.
The US healthcare system can be slow and fragmented. As Veronica Brown’s story illustrates, patients often spend years treating anxiety or joint pain without realizing the root cause is neurological . But there is hope. Early diagnosis allows for early treatment—whether through exercise regimens proven to slow progression, medications like carbidopa-levodopa, or lifestyle adjustments .
And that makes all the difference.What is a hidden symptom of Parkinson’s disease?
When most people think of Parkinson’s disease, they immediately picture hand tremors, shuffling walks, and muscle rigidity. However, the most overlooked symptoms of Parkinson’s are not movement-related at all. Neurologists call these “non-motor symptoms,” and they often begin silently—sometimes years or even decades before the first tremor appears .
The most hidden symptom of Parkinson’s disease is loss of smell (anosmia) . Up to 90% of people with Parkinson’s experience a reduced ability to detect odors—ranging from a complete inability to smell to a subtle dulling of the sense of smell . Most people dismiss this as sinus trouble, allergies, or simply aging. However, this seemingly minor change can be one of the earliest neurological warning signs, often appearing 10 to 20 years before motor symptoms develop .
Why is loss of smell so significant? According to the Braak hypothesis of Parkinson’s progression, the disease process may actually begin in the olfactory bulb (the brain region responsible for smell) and the gut, spreading to the movement-control centers of the brain only later .
Other hidden symptoms that patients and families frequently miss include:
- REM Sleep Behavior Disorder (RBD): Acting out vivid dreams—punching, kicking, shouting, or falling out of bed during sleep. Up to 80% of people with this condition may develop Parkinson’s or a related neurodegenerative disease within 15 years .
- Chronic constipation: Affecting over two-thirds of Parkinson’s patients, this symptom can predate diagnosis by 10 to 20 years .
- Mood changes: Depression and anxiety affect 35% to 45% of individuals with Parkinson’s and may appear before tremors begin .
What are two new early signs of Parkinson’s?
Beyond the well-known constipation and loss of smell, researchers have identified several newer or lesser-known early indicators:
1. Micrographia (Small, Cramped Handwriting)
One of the earliest motor signs of Parkinson’s is a subtle but distinct change in handwriting. Patients begin writing in progressively smaller, more cramped letters, with words crowding together on the page . This condition, called micrographia, reflects the brain’s gradual loss of fine motor control due to dopamine deficiency. Family members may notice that birthday cards, grocery lists, or signature styles have changed significantly—becoming smaller and more difficult to read. Micrographia often appears before other movement symptoms like tremor or stiffness become noticeable .
2. Reduced Arm Swing (Movement Asymmetry)
While walking, most people naturally swing both arms. In early Parkinson’s, one arm may stop swinging or swing with much less amplitude than the other . This asymmetrical movement is a subtle but significant early sign because Parkinson’s typically affects one side of the body more than the other, especially in the early stages . Patients rarely notice this themselves—it is often a family member or friend who observes that “something looks different” when the person walks. This sign can appear years before a resting tremor or slowness becomes evident .
Other emerging early signs being studied include:
- Hypomimia (reduced facial expression): A “masked face” where the person appears serious or depressed despite feeling fine emotionally .
- Diffuse pain: Unexplained shoulder, back, or limb pain that does not respond to typical treatments .
What are the hidden triggers behind Parkinson’s?
While the exact cause of Parkinson’s disease remains unknown, researchers have identified several environmental and genetic factors that may “trigger” or increase the risk of developing the condition. These triggers often operate silently for years before symptoms emerge.
Environmental Triggers
Pesticide and herbicide exposure is one of the most consistently identified environmental risk factors for Parkinson’s . Long-term exposure to certain chemicals—including paraquat, rotenone, and organochlorines—has been linked to a significantly higher risk of developing the disease. These toxins may trigger the misfolding of alpha-synuclein protein, the pathological hallmark of Parkinson’s .
Heavy metal exposure (particularly manganese, lead, and copper) has also been associated with Parkinson’s-like symptoms, especially in occupational settings such as welding or mining .
Gut-Brain Connection
Growing evidence suggests that the gut microbiome may play a triggering role. The Braak hypothesis proposes that Parkinson’s may actually begin in the gut—specifically, that misfolded alpha-synuclein proteins can travel from the enteric nervous system (the “brain of the gut”) up the vagus nerve to the brainstem and eventually into movement-control regions . This explains why chronic constipation is often the very first symptom, appearing decades before any movement issues .
Genetic Triggers
While most Parkinson’s cases are sporadic (without a clear genetic link), about 10% to 15% have a genetic component. Mutations in specific genes—including LRRK2, GBA, and SNCA—significantly increase risk . The GBA gene mutation (associated with Gaucher’s disease) is particularly noteworthy; carriers have a 20- to 30-fold increased risk of developing Parkinson’s.
Other Potential Triggers
- Head trauma: Repeated concussions or traumatic brain injury (TBI) have been associated with increased Parkinson’s risk .
- Certain medications: Antipsychotics and some anti-nausea drugs can induce parkinsonism (symptoms resembling Parkinson’s) .
- Age and sex: Advanced age is the single biggest risk factor, and men are 1.5 times more likely to develop Parkinson’s than women .
It is important to note that having one or more of these triggers does not guarantee someone will develop Parkinson’s. Rather, the disease likely results from a combination of genetic susceptibility and environmental exposures over time .
What is the most noticeable symptom of Parkinson’s disease?
The most noticeable and iconic symptom of Parkinson’s disease is the resting tremor—an involuntary, rhythmic shaking that occurs when the body is relaxed and the limbs are at rest .
What a Resting Tremor Looks Like
Parkinson’s tremors typically have a frequency of 4 to 8 Hz (4 to 8 cycles per second). The classic description is a “pill-rolling” tremor—a circular, back-and-forth movement of the thumb against the fingers, as if rolling a small pill between them . This tremor:
- Appears when the limb is at rest (e.g., hand resting in the lap)
- Diminishes or disappears with voluntary movement (e.g., reaching for a glass)
- Stops completely during sleep
- Usually starts on one side of the body (asymmetric onset)
- May be worsened by stress or anxiety
Approximately 70% to 80% of Parkinson’s patients experience a resting tremor, making it the most common visible motor symptom . However, it is crucial to note that about 20% of people with Parkinson’s never develop a tremor at all—their primary symptoms may be stiffness, slowness, or balance problems instead .
Tremor vs. Other Causes of Shaking
Not every tremor is Parkinson’s. It is essential to distinguish:
| Type | Parkinson’s Tremor | Essential Tremor |
|---|---|---|
| When it occurs | At rest | During action (holding, reaching) |
| Typical location | Hands, feet, jaw | Hands, head, voice |
| Alcohol response | No improvement | May temporarily improve |
| Family history | Less common | Very common |
Other Highly Noticeable Motor Symptoms (The “TRAP” Signs)
Beyond tremor, clinicians look for three other cardinal signs that become very noticeable as the disease progresses :
- Rigidity: Muscle stiffness that feels like “cogwheel” resistance when a doctor moves the patient’s limb—a ratcheting, catch-and-release sensation .
- Akinesia/Bradykinesia: Slowness or poverty of movement. Patients may have difficulty initiating movement, experience “freezing” episodes (feeling stuck in place), and show reduced facial expression (hypomimia) .
- Postural instability: Impaired balance and increased risk of falls. Unlike the other signs, this typically appears later in the disease course .
Early signs of Parkinson’s in females
Parkinson’s affects men 1.5 times more often than women, but the early signs in females can be different and often more subtle. Women may present with more tremor-predominant symptoms (rather than rigidity) and often experience earlier and more significant non-motor symptoms including depression, anxiety, fatigue, and sleep disturbances . Hormonal factors (specifically estrogen) may offer some neuroprotection, potentially explaining why women typically develop Parkinson’s later than men.
5 signs you’ll get Parkinson’s
No single sign definitively predicts Parkinson’s, but the combination of multiple early warning signs significantly increases risk. The five most predictive prodromal signs are :
- REM Sleep Behavior Disorder (acting out dreams)
- Loss of smell (anosmia/hyposmia)
- Chronic constipation (especially if persistent and unexplained)
- Depression or anxiety (without clear cause)
- Asymmetric reduced arm swing or subtle motor changes
Having all three of RBD, smell loss, and constipation creates an “exponentially increased” risk of developing Parkinson’s .
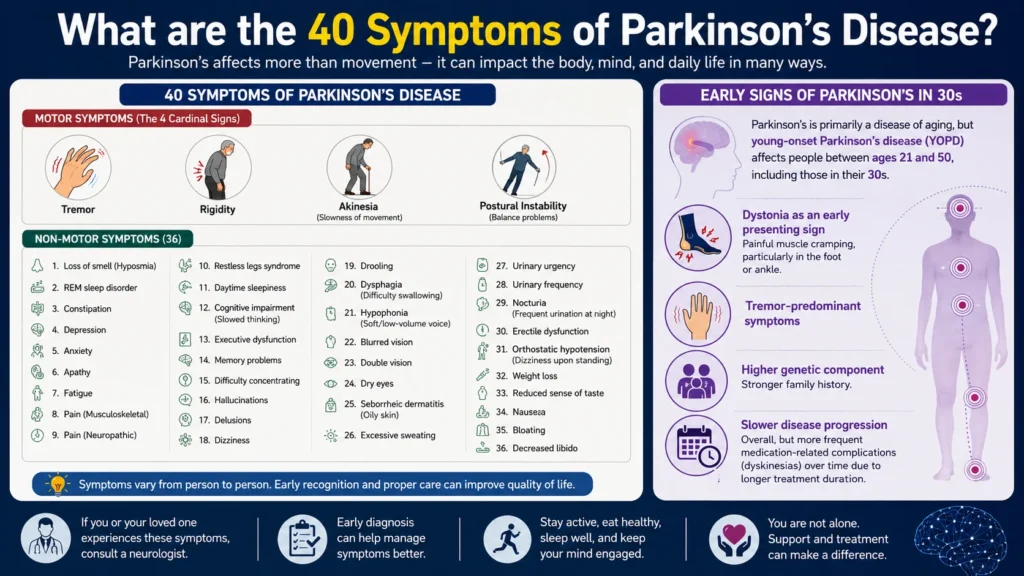
What are the 40 symptoms of Parkinson’s disease
Parkinson’s is remarkably heterogeneous—it affects different people in different ways. Beyond the four cardinal motor signs (tremor, rigidity, akinesia, postural instability), non-motor symptoms can include: loss of smell, REM sleep disorder, constipation, depression, anxiety, apathy, fatigue, pain (musculoskeletal, neuropathic), restless legs syndrome, daytime sleepiness, cognitive impairment (slowed thinking, executive dysfunction), memory problems, drooling, difficulty swallowing (dysphagia), soft/low-volume voice (hypophonia), blurred vision, dry eyes, seborrheic dermatitis (oily skin), excessive sweating, urinary urgency/frequency, erectile dysfunction, orthostatic hypotension (dizziness upon standing), weight loss, and more .
Early signs of Parkinson’s in 30s
Parkinson’s is primarily a disease of aging, but young-onset Parkinson’s disease (YOPD) affects people between ages 21 and 50, including those in their 30s . Early signs in younger patients often include:
- Dystonia (painful muscle cramping, particularly in the foot or ankle) as an early presenting sign
- Tremor-predominant symptoms
- Higher genetic component (stronger family history)
- Slower disease progression overall, but more frequent medication-related complications (dyskinesias) over time due to longer treatment duration
I cured my Parkinson’s disease
There is currently no cure for Parkinson’s disease. Any claim of a “cure” is inaccurate and potentially dangerous . However, Parkinson’s is treatable, and many patients live well with the disease for decades. Standard treatments include:
- Carbidopa-levodopa: The gold-standard medication that replaces dopamine; called one of the most significant breakthroughs in modern medicine
- Dopamine agonists: Medications that mimic dopamine’s effects
- Deep Brain Stimulation (DBS): Surgical implantation of electrodes to regulate abnormal brain activity
- Physical, occupational, and speech therapy: Essential for maintaining function
Some patients report significant symptom improvement with lifestyle modifications (exercise, diet, stress reduction), but these are complementary approaches—not cures.
Early signs of Parkinson’s in males
Men have a higher risk of Parkinson’s overall and may present with more rigidity and bradykinesia (as opposed to tremor) compared to women. Early signs in men include:
- Loss of smell (often unrecognized)
- Constipation
- REM sleep behavior disorder (which disproportionately affects men)
- Reduced arm swing while walking
- Micrographia (small handwriting)
- Erectile dysfunction (as an autonomic symptom)
Early signs of Parkinson’s disease
The earliest signs are predominantly non-motor and appear 5–20 years before diagnosis :
- Loss of smell (most common—90% of patients)
- REM sleep behavior disorder (80% predictive)
- Chronic constipation (2x increased risk)
- Depression and anxiety
- Fatigue and apathy
Later, subtle motor signs emerge: micrographia, reduced arm swing, mild tremor in one hand, softer voice, reduced facial expression, and slight slowness in daily activities.
Parkinson’s disease causes, symptoms and treatment
Causes: Combination of genetic susceptibility (10-15% familial), environmental exposures (pesticides, heavy metals, head trauma), age (primary risk factor), and sex (male predominance) .
Symptoms: Divided into motor (tremor, rigidity, bradykinesia, postural instability) and non-motor (anosmia, RBD, constipation, depression, anxiety, fatigue, cognitive changes, autonomic dysfunction) .
Treatment: No cure exists, but symptomatic management includes: levodopa/carbidopa, dopamine agonists, MAO-B inhibitors, anticholinergics, amantadine, deep brain stimulation surgery, and multidisciplinary rehabilitation .
Summary Table: Key Parkinson’s Early Signs
| Symptom | Type | Lead Time Before Diagnosis | Prevalence |
|---|---|---|---|
| Loss of smell (anosmia) | Non-motor | 10-20 years | 90% of patients |
| REM Sleep Behavior Disorder | Non-motor | 10-15 years | 80% predictive |
| Chronic constipation | Non-motor | 10-20 years | 66%+ of patients |
| Depression/Anxiety | Non-motor | 5-10 years | 35-45% |
| Micrographia (small writing) | Motor | Early stage | Common |
| Reduced arm swing | Motor | Early stage | Common |
| Resting tremor | Motor | At diagnosis | 70-80% |
When to See a Doctor
No single symptom alone confirms Parkinson’s disease. However, if you or a loved one experiences multiple of these warning signs—especially the combination of REM sleep behavior disorder, loss of smell, and chronic constipation—consult a neurologist, preferably one specializing in movement disorders . Early detection does not change the underlying disease progression, but it allows for earlier symptomatic treatment, better quality of life, and more time to plan for future care needs .
FAQ
#1: Hidden Symptoms and Early Signs of Parkinson’s Disease
Many people think Parkinson’s only causes shaking, but the earliest signs are often subtle and easy to miss. Hidden symptoms can appear years before movement problems begin. These may include loss of smell, constipation, vivid dreams with body movements during sleep, anxiety, depression, fatigue, or unusually small handwriting. Some people notice stiffness in one shoulder, softer speech, or slower walking long before a diagnosis is made. Early detection is important because treatment and lifestyle changes may help manage symptoms more effectively and improve quality of life.
#2: Triggers, Most Noticeable Symptom, and Treatment of Parkinson’s Disease
The exact cause of Parkinson’s disease is still not fully understood, but experts believe it develops from a combination of aging, genetic factors, environmental toxin exposure, and changes in brain chemistry. The most noticeable symptom is usually a resting tremor, especially in one hand, though slowness of movement and muscle stiffness are also very common. Treatment may include medications that increase dopamine levels, physical therapy, speech therapy, regular exercise, and in some cases advanced procedures like deep brain stimulation. While Parkinson’s currently has no cure, many people manage symptoms successfully for years with proper medical care and lifestyle support.
⚠️ Medical Disclaimer
This article is for informational and educational purposes only and does not constitute medical advice. The content is not intended to be a substitute for professional medical diagnosis, treatment, or personalized care. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition, including Parkinson’s disease or its symptoms. Never disregard professional medical advice or delay seeking it because of something you have read here. If you think you may have a medical emergency, call your doctor or emergency services immediately.